Courtesy: Thurston Gehrke,m Ashok Shyam, IORG, OrthoTV
Periprosthetic Joint Infection (PJI): Diagnosis and Management
Overview
- Periprosthetic Joint Infection (PJI) is a major complication after:
- Total hip replacement
- Total knee replacement
Clinical Importance
- Difficult to diagnose
- Challenging to treat
- Significant impact on:
- Patient outcomes
- Healthcare systems
Challenges in Diagnosis
Limitations of Traditional Markers
- C-reactive protein (CRP):
- May be normal in some infected cases
- Erythrocyte sedimentation rate (ESR):
- Often unreliable
Biological Challenges
- Bacteria may:
- Hide within cells
- Reside in bone canaliculi
- Form biofilms — evade detection
Modern Diagnostic Approach
- Use of standardized algorithms:
- International Consensus Meeting (ICM) criteria
Clinical Scenario (Typical Presentation)
- Increasing joint pain after a pain-free period
- Suspicion of infection — further evaluation required
Aspiration Technique
- Performed under:
- Fluoroscopy
- Strict sterile conditions
Diagnostic Findings
- Elevated:
- Synovial cell count
- Polymorphonuclear (PMN) percentage
Key Diagnostic Modalities
1. Synovial Fluid Analysis
Parameters
- Cell count
- PMN percentage
- Alpha defensin
- Leukocyte esterase
Important Tool
- Leukocyte esterase test:
- Sensitive
- Cost-effective
2. Culture and Biopsy
Indications
- Culture-negative cases
Approach
- Repeat aspiration
- Open biopsy
3. Molecular Diagnostics
Techniques
- Broad-range 16S PCR
- Multiplex PCR
- Next-generation sequencing (NGS)
Advantages of NGS
- Detects polymicrobial infections
- Identifies resistance genes
Limitations
- High cost
- Complex interpretation
Treatment Approach
Core Principle
- Multidisciplinary management is essential
Team Involves
- Orthopaedic surgeon
- Microbiologist
- Infectious disease specialist
Surgical Strategies
1. Two-Stage Exchange (Conventional Standard)
Steps
- Implant removal
- Debridement
- Antibiotic spacer
- Delayed reimplantation
2. One-Stage Exchange (Emerging Trend)
Features
- Single surgery
- Removal + reimplantation in same sitting
Advantages
- Reduced morbidity
- Faster recovery
Requirement
- Known organism
- Good soft tissue condition
Key Surgical Principles
- Thorough debridement
- Appropriate antibiotic therapy
- Use of antibiotic-loaded cement
- Strict aseptic technique:
- Re-draping
- New instruments during reimplantation
Implant Considerations
Hip
- Dual mobility cups — reduce instability
Knee
- Hinged prosthesis:
- In cases of extensive debridement
Evidence and Outcomes
One-Stage vs Two-Stage
- Comparable or better outcomes in selected patients
- High success rates:
- Infection eradication
- Reimplantation
Factors Affecting Success
- Identification of organism
- Antibiotic sensitivity
- Patient comorbidities
- Adequacy of debridement
Key Take-Home Messages
- Diagnosis requires a combined approach:
- Clinical
- Laboratory
- Imaging
- Highly useful tests:
- Leukocyte esterase
- PMN percentage
- Culture-negative cases:
- Repeat aspiration or biopsy
- Multidisciplinary care improves outcomes
- One-stage exchange is an effective option in selected patients

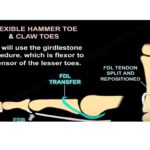
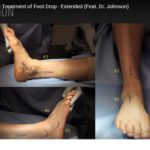
What about 2ndry deformity such as flatfoot which occur in PTTD after transferring it for dorsiflexion????