Courtesy: Dr Mette Andersen, Tromso, Norway
High Ankle Sprains (Syndesmotic Injuries): Evaluation & Management
Overview
High ankle sprains involve injury to the distal tibiofibular syndesmosis and are frequently missed.
Clinical Importance
Missed diagnosis may lead to:
- Delayed return to sport
- Chronic instability
- Soft tissue impingement
- Post-traumatic osteoarthritis
Nearly 80% of ankle osteoarthritis is post-traumatic
Case Example
Typical Scenario
- Athlete: Junior kickboxer
- Mechanism:
- Hyper-dorsiflexion
- External rotation
- Axial loading
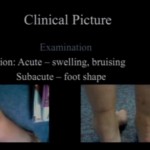
Clinical Findings
- Positive squeeze test
- Tenderness:
- Deltoid ligament
- Interosseous membrane
Imaging
- X-ray: Normal
- MRI findings:
- AITFL injury
- Interosseous membrane edema
- No PITFL tear
- No deltoid ligament injury
- No diastasis
Key Clinical Challenge
Primary Objectives
- Avoid missed diagnosis
- Differentiate between:
- Stable injuries
- Unstable injuries
Classification: West Point System
Grade 1
- Partial AITFL tear
- Stable
Grade 2 (Most Challenging)
- Complete AITFL rupture
- Partial interosseous ligament injury
- No diastasis on X-ray
- Possible subtle instability
Grade 3
- Complete syndesmotic disruption
- Clear diastasis
- Unstable
Epidemiology
Common in
- Collision sports
- Skiing and hockey
Incidence
- Approximately 20% of ankle sprains (MRI-detected)
- 13–18% in elite football
Risk
- 14 times higher during matches compared to training
Mechanism of Injury
Typical Pattern
- External rotation combined with dorsiflexion
- Pronated ankle
Key Factor
- Fixed forefoot increases severity
Clinical Examination
General Principle
No single test is definitive.
Most Useful Tests
Squeeze Test
- Highest specificity
External Rotation Test
- Good sensitivity
Less Reliable Tests
- Cotton test
- Fibular translation test
Additional Finding
- Tenderness along the interosseous membrane
- Greater proximal spread indicates more severe injury
Imaging Modalities
X-ray
- Detects fractures and gross diastasis
- May miss subtle instability
CT Scan
- More sensitive than X-ray
- Requires bilateral comparison
- Static assessment
Weight-Bearing CT
- Promising but limited availability
Ultrasound
- Dynamic and cost-effective
- Operator dependent
MRI (Best Imaging Modality)
Accuracy
- Sensitivity and specificity: 95–100%
Findings
- AITFL and PITFL injuries
- Interosseous ligament edema
- Associated intra-articular injuries
Limitation
- Does not directly assess instability
Important MRI Signs
- AITFL discontinuity
- Interosseous ligament edema
- PITFL injury
- Posterior malleolar edema
- Periosteal stripping
- “Broken ring of fire” sign
Associated Injuries
Incidence
- Up to 50% of cases
Types
- Loose bodies
- Cartilage lesions
Gold Standard
Arthroscopy
Advantages
- Confirms instability
- Direct visualization
- Allows treatment of associated lesions
Signs of Instability
- Syndesmotic widening > 2–3 mm
- Positive drive-through sign
Indicators of Instability
- Mechanism: dorsiflexion with external rotation
- Positive squeeze test or external rotation test
- Deltoid ligament injury
- PITFL injury on MRI
Management
Conservative Treatment (Stable Injuries)
Protocol
- 3 weeks non-weight-bearing
- Followed by 3 weeks in a walking boot
Grade 1 Injuries
- Faster recovery (approximately 3 weeks)
Surgical Treatment (Unstable Injuries)
Indications
- Grade 3 injuries
- Confirmed instability
Options
- Syndesmotic screw fixation
- Suture button device
- With or without ligament repair
Screw vs Suture Button
Suture Button
- Better functional outcomes
- Lower malreduction rates
- Reduced long-term osteoarthritis risk
Key Principle
Accurate reduction is more important than implant choice
Complications
- Joint stiffness
- Malreduction (up to 40%)
- Implant irritation
- Fractures (especially in osteoporotic bone)
Rehabilitation Protocol
- Boot immobilization: approximately 4 weeks
- Weight-bearing: after 2 weeks if tolerated
- Range of motion: begin at 10 days
- Proprioception training: from week 3
- Impact activities: from week 5
Return to Sport
- Conservative management: approximately 6 weeks
- Surgical management: 9–14 weeks
Negative Predictors
- Grade 3 injury
- Age above 25 years
- Associated cartilage injury
Key Takeaways
- Maintain high suspicion for syndesmotic injury
- Use a combination of clinical tests and imaging
- MRI is essential but does not confirm instability
- Arthroscopy remains the gold standard
- Stable injuries are treated conservatively
- Unstable injuries require surgical stabilization
- Quality of reduction determines outcome
Clinical Pearls
- Most reliable clinical indicators:
- Squeeze test
- Local ligament tenderness
- Chronic cases:
- Taping or stabilization tests may be useful
- Deltoid ligament:
- Increasingly recognized as a key stabilizer
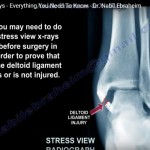
- Weight-bearing X-ray:
- Limited role in detecting subtle instability


Leave a Reply