Courtesy: Amr Abdelgawad, Maimonaides Medical Centre, NY, USA
- Types of Bone Histology
Organized Bone (Lamellar Bone)
Cortical Bone
– Forms the cortex of long bones.
– Located in the shaft of bones such as the femur and tibia.
– Dense with low porosity.
– Lower surface area for the same bone volume.
– Stronger and stiffer.
– Lower metabolic activity.
Cancellous Bone (Trabecular Bone)
– Located mainly in the metaphysis of long bones.
– Highly porous.
– Larger surface area.
– Less stiff compared to cortical bone.
– Higher metabolic activity.
Woven Bone
– Disorganized bone structure.
– Seen during early fracture healing and callus formation.
- Bone Structure and Chemistry
Inorganic (Mineral) Component
– Makes up about 60–70 percent of bone.
– Mainly calcium and phosphate.
– Present primarily as hydroxyapatite crystals.
– Chemical composition: Calcium10(PO4)6(OH)2.
Organic Matrix
– About 30 percent of bone.
– Mainly composed of Type I collagen.
– Type I collagen accounts for about 90 percent of the organic matrix.
Water
– Approximately 5–8 percent of bone.
- Bone Cells
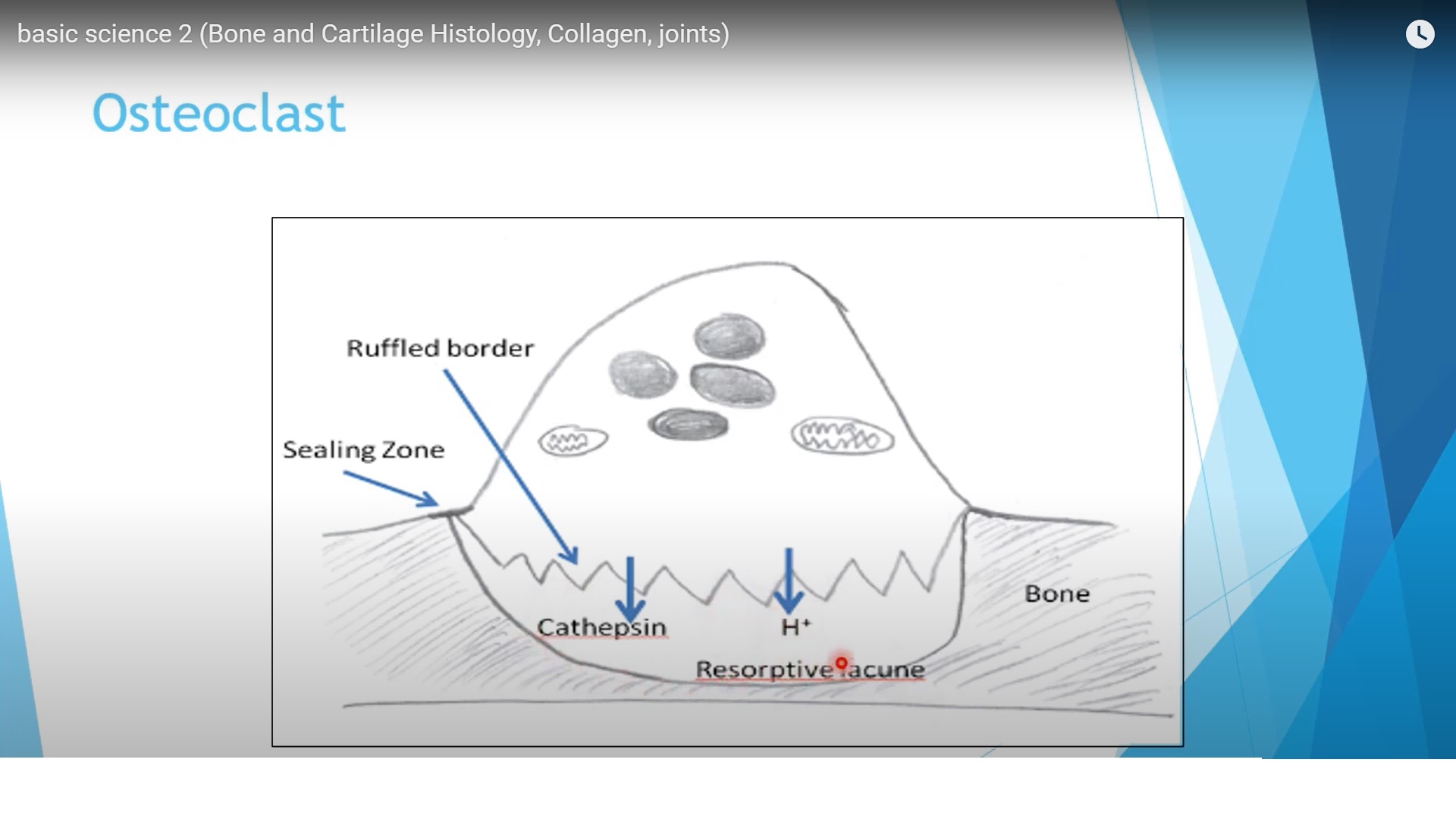
Osteoclast
– Responsible for bone resorption.
– Derived from hematopoietic lineage.
– Develop from monocyte–macrophage cells.
– Multinucleated giant cells with ruffled border and sealing zone.
– Carbonic anhydrase generates hydrogen ions to dissolve mineral.
– Cathepsin and matrix metalloproteinases degrade organic matrix.
RANK–RANKL–OPG Pathway
– RANK present on osteoclast precursors.
– RANK ligand produced by osteoblasts.
– Interaction increases osteoclast formation and bone resorption.
– Osteoprotegerin blocks RANK ligand and reduces osteoclast formation.
– Denosumab acts similarly by blocking RANK ligand.
Factors Increasing RANK Ligand
– Interleukin 1
– Corticosteroids
– Vitamin D
– Continuous hyperparathyroidism
Osteoblast
– Derived from mesenchymal stem cells.
– Responsible for bone formation and matrix production.
– Produces osteocalcin.
– Osteocalcin is vitamin K dependent and produced only by mature osteoblasts.
– Major non collagenous protein in mature bone.
– Marker of bone formation.
Important Gene
– RUNX2 (CBFA1)
– Controls differentiation of mesenchymal stem cells into osteoblasts.
– Mutation leads to cleidocranial dysplasia.
Osteocyte
– Derived from osteoblasts embedded in bone matrix.
– Less metabolically active.
– Communicate through canaliculi.
– Sense mechanical stress and regulate remodeling.
- Growth Plate (Physis)
Responsible for longitudinal growth of long bones.
Present only in growing skeleton.
Zones
Resting Zone
– Small chondrocytes.
– Large extracellular matrix.
– Low oxygen and metabolic activity.
Proliferative Zone
– Rapid chondrocyte division.
– Cells arranged in columns.
– High extracellular matrix synthesis.
Hypertrophic Zone
– Chondrocytes enlarge.
– Subdivided into maturation, degeneration, and provisional calcification.
Most physeal fractures occur in the zone of provisional calcification.
Supporting Structures
Perichondral Ring of LaCroix
– Provides mechanical support.
Groove of Ranvier
– Responsible for appositional growth.
- Collagen
– Triple helical protein structure.
– Three alpha chains.
– Sequence pattern Glycine–X–Y.
– X and Y commonly proline or hydroxyproline.
Types of Collagen
Type I
– Main collagen in bone.
– Also present in skin and annulus fibrosus.
Type II
– Main collagen in cartilage.
Type IX and XI
– Minor collagen types in cartilage.
Type X
– Present in hypertrophic chondrocytes during endochondral ossification.
- Articular Cartilage
Cells
– Chondrocytes (about 2 percent).
Extracellular Matrix
– About 98 percent.
– Components: water, Type II collagen, proteoglycans.
- Layers of Articular Cartilage
Superficial Zone
– 10–15 percent thickness.
– Collagen parallel to surface.
– Highest tensile strength.
– Highest water and collagen content.
– Lowest proteoglycan.
Middle Zone
– Transitional layer.
Deep Zone
– Collagen perpendicular to surface.
– Highest proteoglycan content.
– Cells arranged in columns.
Calcified Zone
– Anchors cartilage to subchondral bone.
– Separated from deep zone by tidemark.
- Glycosaminoglycans and Proteoglycans
Glycosaminoglycans
– Linear polysaccharides.
– Examples: chondroitin sulfate, keratan sulfate.
Proteoglycan Monomer
– Core protein attached to glycosaminoglycan chains.
Proteoglycan Aggregate
– Multiple monomers attached to hyaluronic acid via link proteins.
Function
– Bind water and provide resistance to compression.
- Chondroprotective Factors
– Transforming growth factor beta
– Bone morphogenetic proteins 2 and 7
– Insulin like growth factor
– Glucosamine
Effects
– Increase collagen and proteoglycan synthesis.
- Cartilage Degrading Factors
– Interleukin 1
– Tumor necrosis factor
– Matrix metalloproteinases
– Cyclooxygenase enzymes
Effects
– Increase cartilage degradation.
– Decrease proteoglycan synthesis.
- Aging vs Osteoarthritis Changes
Aging
– Decreased water content.
– Increased stiffness.
– Decreased proteoglycan synthesis.
– Decreased chondrocyte number.
Osteoarthritis
– Increased water content.
– Softer cartilage.
– Increased proteoglycan turnover.
– Increased chondrocyte number.
- Synovial Joint
Synovium Layers
– Intimal layer
– Subintimal connective tissue layer
Cell Types
Type A Cells
– Macrophage-like
– Phagocytosis
Type B Cells
– Fibroblast-like
– Produce synovial fluid
Synovial Fluid
– Contains hyaluronic acid
– Low protein concentration
– Non-Newtonian fluid behavior
- Joint Lubrication
Elastohydrodynamic Lubrication
– Deformation of surfaces with fluid film lubrication.
Boundary Lubrication
– Occurs when fluid film is minimal.
– Lubrication via surface molecules.
- Lubricin and Superficial Zone Protein
– Glycoproteins produced by superficial zone chondrocytes.
– Important for boundary lubrication.
– Hyaluronic acid interacts with lubricin to reduce friction.


Leave a Reply