Courtesy: Prof Nabil Ebraheim, University of Toledo, Ohio, USA
Overview
The acetabulum forms the socket of the hip joint and articulates with the femoral head.
For clinical and surgical understanding, it is divided into two structural columns, which are essential for:
- Interpreting acetabular fractures
- Planning surgical approaches
Several important vessels and nerves lie in close proximity and are at risk during trauma and surgery
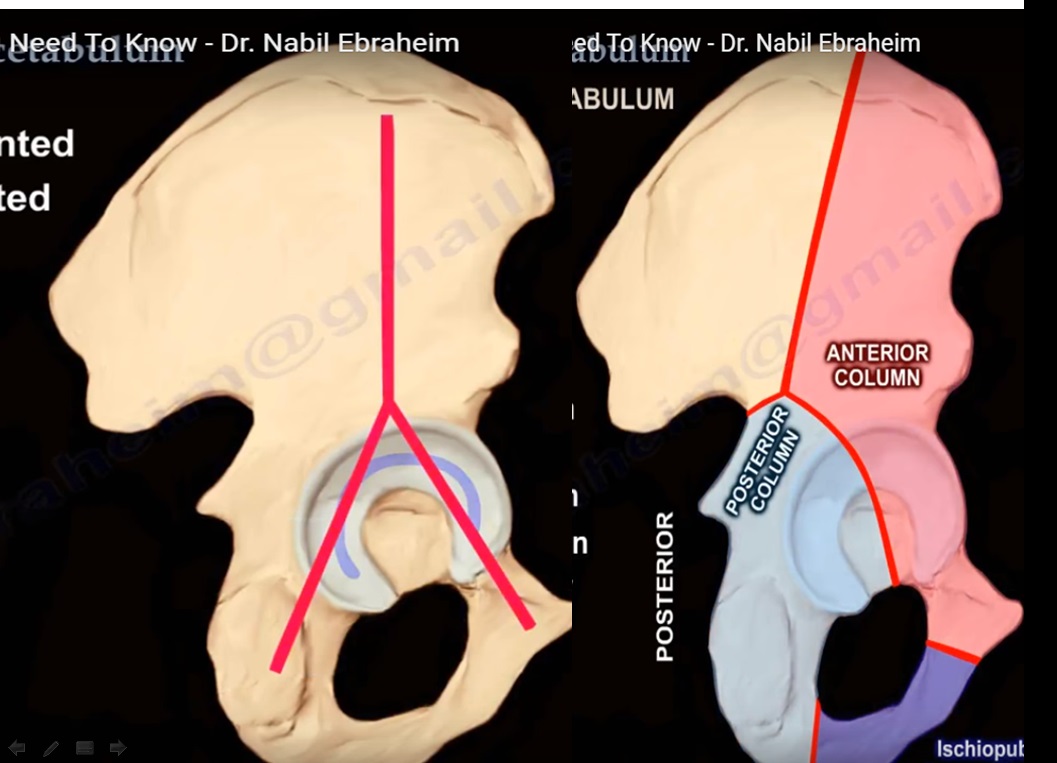
Columns of the Acetabulum
Structural Concept
The acetabulum is divided into:
- Anterior column
- Posterior column
These columns form the load-bearing framework of the hip joint.
Anterior Column
Components
- Anterior ilium
- Anterior acetabular wall
- Weight-bearing dome
- Superior pubic ramus
Function
- Provides anterior and superior support
Posterior Column
Extent
- From obturator foramen
- Through posterior acetabular dome
- To greater sciatic notch
Function
- Provides posterior structural stability
Ischiopubic Ramus
Formation
- Inferior pubic ramus
- Inferior ramus of ischium
Role
- Forms the inferior border of the obturator foramen
Pelvic Structural Orientation
- The acetabulum can be visualized as an inverted “Y” structure
- Represents the relationship between anterior and posterior columns
Vascular Anatomy Around the Acetabulum
Obturator Artery
Origin
- Anterior division of the internal iliac artery
Course
- Travels within pelvis – passes through obturator canal
Branches
- Anterior branch
- Posterior branch
- Forms a vascular ring around the obturator membrane
Acetabular Branch
- Travels through ligament of the femoral head
- Supplies a small portion of the femoral head
Corona Mortis
Definition
- Vascular connection between:
- Obturator system (internal iliac)
- External iliac system (often via inferior epigastric vessels)
Location
- 3–7 cm from pubic symphysis
- Posterior and superior to the superior pubic ramus
Clinical Importance
- At risk during:
- Pelvic trauma
- Fracture surgery
- Ilioinguinal approach
Injury may cause severe hemorrhage
Superior Gluteal Artery
Course
- Passes through the greater sciatic notch
Clinical Relevance
- May be injured in:
- Posterior column fractures
- Posterior surgical approaches
Risk increases with excessive retraction
Medial Femoral Circumflex Artery
Importance
- Primary blood supply to the femoral head
Risk of Injury
- Hip dislocation
- Improper surgical dissection (e.g., detaching quadratus femoris incorrectly)
Surgical Tip
- Preserve a small tendon cuff to protect the deep branch
Nerve Anatomy Related to the Acetabulum
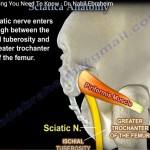
Sciatic Nerve
Relationship
- Lies close to the posterior acetabulum
Incidence of Injury
- Most common nerve injury in acetabular trauma
- Occurs in ~10% of hip dislocations
Clinical Examination
- Ankle dorsiflexion
- Toe dorsiflexion
- Sensation over dorsum of foot
Peroneal division most commonly affected
Surgical Precautions
- Keep:
- Hip extended
- Knee flexed
Reduces nerve tension
Anatomical Relations
- Posterior to obturator internus
- Inferior to piriformis
Variations may occur (e.g., nerve splitting)
Protection
- Obturator internus acts as a buffer during retraction
Superior Gluteal Nerve
Location
- Near greater sciatic notch
Risk
- Injury if dissection extends >5 cm above greater trochanter
Consequence
- Weakness of:
- Gluteus medius
- Gluteus minimus
Leads to Trendelenburg gait
Inferior Gluteal Nerve
Function
- Supplies gluteus maximus
Risk
- Injury during posterior approaches
Lateral Femoral Cutaneous Nerve
Course
- Passes beneath inguinal ligament
- ~2 cm medial to ASIS
Risk
- Injury during ilioinguinal approach
Clinical Effect
- Sensory disturbance over lateral thigh
Summary Points
- Acetabulum consists of anterior and posterior columns
- Forms an inverted Y-shaped structure
- Key vessels:
- Obturator artery
- Corona mortis
- Superior gluteal artery
- Medial femoral circumflex artery
- Key nerves at risk:
- Sciatic nerve
- Superior gluteal nerve
- Inferior gluteal nerve
- Lateral femoral cutaneous nerve
Clinical Takeaway
A thorough understanding of:
- Column anatomy
- Vascular relations
- Nerve proximity
is essential for:
- Accurate fracture management
- Safe surgical approaches
- Avoidance of major complications

Leave a Reply