Courtesy: Prof Alfonso Manzotti, Luigi Sacco Hospital, Milan, Italy
Patient Profile Commonly Associated with PJI
Periprosthetic joint infection is more frequently encountered in patients with:
-
Highly complex surgical cases
-
Multiple comorbidities (pluripatological patients)
-
History of multiple surgical procedures
-
Poor treatment compliance
The Clinical Problem
-
A painful total knee arthroplasty (TKA) without an identifiable mechanical cause should be considered infected until proven otherwise.
-
Patient-reported outcomes are often poor:
-
Only 23% report satisfaction
-
Approximately 18% report complete dissatisfaction
-
Epidemiology and Microbiology
Common Causative Organisms
-
Coagulase-negative staphylococci: 30–43%
-
Staphylococcus aureus: 12–23%
-
Streptococci: 9–10%
-
Enterococci: 3–7%
Infection Rates
-
Primary joint replacement (first 2 years):
-
Hip and shoulder: <1%
-
Knee: <2%
-
Elbow: <9%
-
-
Revision arthroplasty:
-
Infection rates significantly higher, reported up to 40%
-
Classification of PJI
Early PJI (< 6 months)
-
Usually caused by high-virulence organisms
-
Common pathogens:
-
Staphylococcus aureus
-
Gram-negative bacteria
-
-
Often related to:
-
Perioperative contamination
-
Early postoperative hematogenous or lymphatic spread
-
Routes of Infection
-
Perioperative:
Inoculation during surgery or immediately postoperatively -
Hematogenous:
Spread via blood or lymphatics from a distant infectious focus -
Contiguous:
Direct extension from adjacent infection
(e.g., penetrating trauma, pre-existing osteomyelitis, skin or soft-tissue infection)
Evolution of PJI Diagnostic Criteria
-
2004 – Zimmerli criteria
-
2010 – AAOS guidelines
-
2013 – IDSA guidelines
-
2018 – International Consensus Meeting
-
2021 – European Bone and Joint Infection Society (EBJIS)
Diagnostic Criteria for PJI
Major Criteria
-
Sinus tract communicating with the prosthesis
-
Isolation of the same pathogen from two separate tissue or fluid samples
Minor Criteria
PJI is diagnosed if three of the following five are present:
-
Elevated ESR and CRP
-
Synovial WBC count >3,000 cells/µL or positive leukocyte esterase
-
Synovial PMN percentage >80%
-
Isolation of a microorganism in a single culture
-
5 WBCs per high-power field in 5 high-power fields on histology
Diagnostic Protocol for Suspected PJI
-
Clinical history and physical examination
-
Blood tests and joint aspiration
-
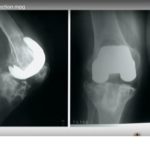
Standard radiographs
-
Wedge-shaped bone resorption
-
Periosteal scalloping
-
-
Advanced imaging (when indicated):
-
Nuclear medicine studies
-
CT or MRI
-
-
Further specialized investigations in atypical cases
Blood Tests and Joint Aspiration
Serum Biomarkers (Minor Criteria)
-
C-reactive protein (CRP)
-
D-dimer
-
Plasma fibrinogen (excellent biomarker)
-
ESR (note: normal in ~4% of PJIs)
Serum-negative PJI:
Approximately 4% of patients have normal ESR and CRP.
Synovial Fluid (SF) Analysis
Used by ~97% of surgeons, but culture-negative infections occur in 20–40%.
Components of SF Analysis (5-in-1)
-
Aerobic and anaerobic culture
-
Leukocyte esterase
-
Synovial WBC count
-
Synovial PMN percentage
-
Alpha-defensin (routine use not mandatory)
Diagnostic Thresholds for Synovial WBC and PMN%
| Condition | WBC Count |
|---|---|
| Acute hip PJI | >12,800 |
| Chronic hip PJI | >3,966 |
| Acute knee PJI | >10,700 |
| Chronic knee PJI | >3,000 |
-
Synovial calprotectin is emerging as a useful marker for chronic PJI.
Tips and Tricks for Synovial Fluid Analysis
-
Use pre-prepared aspiration sets
-
Always perform optical microscopy
-
Aspirate at least 15 mL of fluid:
-
5 mL for anaerobic culture
-
5 mL for aerobic culture
-
2 mL for cell count
-
2 mL for leukocyte esterase
-
1 mL for alpha-defensin
-
Second-Level Investigations
Ultrasound
-
Pros:
Low cost, widely available, useful for soft-tissue monitoring and biopsy guidance -
Cons:
Low sensitivity and specificity
CT Scan
-
Pros:
Useful for bone biopsy guidance -
Cons:
Metal artefacts, radiation exposure, contrast risks, lower accuracy than MRI
MRI
-
Pros:
High diagnostic accuracy with modern metal-artifact-reduction sequences
Radiation-free -
Cons:
Peri-implant edema may cause false positives
Nuclear Medicine Imaging
Tc-MDP / HDP Bone Scan
-
High sensitivity
-
Low specificity
-
Useful as a screening tool in chronic infections
99mTc-HMPAO / In-Oxine WBC Scan
-
High sensitivity and specificity
-
Particularly useful in acute infection
-
Can be combined with bone marrow scan
-
Limitations: availability, radiation, blood handling
FDG-PET/CT
-
High sensitivity
-
Low specificity
-
High radiation dose
-
Difficult interpretation and high cost
Intraoperative Investigations
-
Obtain 3–5 sterile tissue samples
-
Avoid swabs
-
Use blood culture bottles (e.g., BACTEC)
-
Sonication of removed implants:
-
More sensitive than standard periprosthetic tissue cultures
-
Similar specificity
-
-
DTT and sonication have similar sensitivity and outperform standard cultures
Advanced Microbiological Techniques
-
Microbial DNA PCR (panels of 8–20 organisms)
-
Next-generation sequencing (NGS)
-
Particularly helpful in culture-negative infections
Take-Home Messages
-
Diagnosis of PJI is never presumptive
-
Always start with clinical history and examination
-
Apply standardized PJI diagnostic criteria
-
Follow a stepwise, protocol-based approach
-
Multidisciplinary collaboration improves accuracy
-
Proceed to advanced diagnostics only when results are inconclusive
-
Emerging technologies will enhance diagnostic precision in the future


Leave a Reply