Courtesy: Prof Nabil Ebraheim, University of Toledo, Ohio, USA
Ulnar Nerve: High-Yield Clinical Facts
Overview
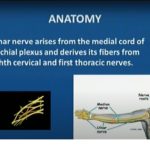
The Ulnar Nerve originates primarily from the C8–T1 nerve roots of the brachial plexus. It is responsible for sensation in the medial hand and motor supply to many intrinsic hand muscles.
Common Sites and Causes of Ulnar Nerve Compression
Most Common Site
The most common site of compression is the cubital tunnel, especially between the two heads of the flexor carpi ulnaris (FCU).
Other Causes
Additional causes of ulnar nerve compression include:
- Anconeus epitrochlearis muscle
- Cubital tunnel narrowing
- Osteophytes or deformity around the elbow
- Ganglion cysts
- Arcade of Struthers
- Trauma or valgus instability
- Repetitive elbow flexion
Root Value and Clinical Importance
Root Value
The ulnar nerve arises mainly from:
- C8–T1
Relation to Horner Syndrome
These same roots may also be involved in lesions producing Horner Syndrome.
Presence of Horner syndrome in a brachial plexus injury suggests a poor prognosis, usually indicating lower trunk or root avulsion involvement.
First Dorsal Interosseous Muscle
Clinical Importance
The first dorsal interosseous muscle is supplied by the ulnar nerve.
Findings
- Wasting of this muscle indicates ulnar nerve palsy
- Visible wasting in the first web space suggests chronic denervation and poorer prognosis
Thenar vs Interosseous Wasting
Thenar Wasting
Associated mainly with median nerve compression, especially Carpal Tunnel Syndrome.
Interosseous Wasting
Associated with ulnar nerve lesions.
Martin–Gruber Anastomosis
Definition
A communicating branch between the median nerve and ulnar nerve in the forearm.
Importance
It can:
- Alter clinical findings
- Confuse nerve conduction studies and EMG interpretation
- Produce unexpected muscle preservation patterns
Cubital Tunnel and Elbow Flexion
Key Fact
Elbow flexion significantly decreases cubital tunnel volume and increases pressure on the ulnar nerve.
Clinical Relevance
- Prolonged elbow flexion may worsen symptoms
- Excessive mobile phone use may aggravate cubital tunnel syndrome
Dorsal Cutaneous Branch of the Ulnar Nerve
Important Sensory Branch
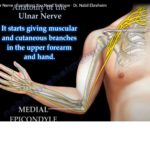
The dorsal cutaneous branch arises in the forearm proximal to the wrist.
High Ulnar Nerve Lesion (At/Above Elbow)
Causes:
- Sensory loss over dorsal medial hand
- Sensory loss over medial 1½ fingers dorsally
Low Ulnar Nerve Lesion (At Wrist)
Usually spares dorsal sensation because the dorsal cutaneous branch has already originated proximally.
Sensory Distribution
Palmar Cutaneous Branch
Supplies sensation to the:
- Hypothenar eminence
Superficial Terminal Branch
Supplies sensation to:
- Little finger
- Medial half of ring finger
Ulnar Claw Hand
Low Ulnar Nerve Lesion
Lesions at the wrist or distal forearm produce:
- Clawing of the ring and little fingers
- Hyperextension at MCP joints
- Flexion at IP joints
This occurs because the lumbricals and interossei are paralyzed while FDP to ring and little fingers remains intact.
High Ulnar Nerve Lesion
May produce:
- Less clawing (“ulnar paradox”)
- More sensory loss
Because FDP to the medial fingers is also weak.
Claw Hand vs Benediction Sign
Ulnar Claw
Seen at rest involving:
- Ring finger
- Little finger
Benediction Sign
Occurs during attempted fist-making in median nerve injury.
The patient cannot flex:
- Index finger
- Middle finger
Role of Flexor Digitorum Profundus (FDP)
Innervation
- Medial half (ring and little finger): ulnar nerve
- Lateral half (index and middle finger): median nerve
This explains the difference between high and low ulnar nerve lesions.
Wartenberg Sign
Definition
Persistent abduction of the little finger due to weakness of:
- Palmar interossei (adductors)
Mechanism
The extensor digiti minimi remains unopposed, causing abduction.
Wartenberg Syndrome
Different Condition
Wartenberg Syndrome is unrelated to ulnar nerve palsy.
It is caused by compression of the superficial radial nerve between:
- Brachioradialis
- Extensor carpi radialis longus
Commonly aggravated by:
- Tight watches
- Bracelets
- Handcuffs
Arcade of Struthers vs Ligament of Struthers
Arcade of Struthers
Potential site of ulnar nerve compression proximal to the elbow.
Ligament of Struthers
A fibrous band extending from a supracondylar spur that may compress the median nerve.
Froment Sign
Test
The patient attempts to hold a paper between thumb and index finger.
Positive Froment Sign
Because the adductor pollicis (ulnar nerve) is weak, the patient compensates by flexing the thumb IP joint using:
- Flexor pollicis longus (median nerve)
This produces thumb flexion during pinch.
Froment Sign vs Anterior Interosseous Nerve (AIN) Palsy
Anterior Interosseous Nerve Palsy
The patient cannot make a normal “OK” sign because of weakness of:
- Flexor pollicis longus
- FDP to index finger
The pinch becomes flattened instead of circular.
Froment Sign
The patient can still flex the thumb, but does so abnormally to compensate for ulnar nerve weakness.
Tinel Sign at the Cubital Tunnel
Technique
Tapping over the cubital tunnel reproduces tingling along the ulnar nerve distribution.
Clinical Use
Supports diagnosis of:
- Cubital tunnel syndrome
- Ulnar neuritis
Differential Diagnosis of Ulnar Symptoms
Conditions that may mimic cubital tunnel syndrome include:
- Cervical radiculopathy (especially C8–T1)
- Thoracic outlet syndrome
- Double crush syndrome
- Lower brachial plexopathy
Sensory Testing
Quick Bedside Test
Check sensation over:
- Little finger
- Medial half of ring finger
Useful in postoperative or trauma settings.
Supracondylar Fracture and Nerve Injury
Extension-Type Supracondylar Fracture
Most commonly associated with:
- Median nerve injury
- Anterior interosseous nerve injury
Flexion-Type Supracondylar Fracture
More commonly associated with:
- Ulnar nerve injury
Flexion-type injuries are less common and may require open reduction more frequently.
Related Posts
-
Ulnar Nerve Palsy
Courtesy: Dr GC Basavaraja, Davengere, India
-
Ulnar Nerve-Clinical Examination
Courtesy: Prof Nabile ebraheim, University of Toledo, Ohio, USA
-
Ulnar Nerve Anatomy
Courtesy: Prof Nabil Ebraheim, University of Toledo, Ohio, USA ORIGIN AND COURSE The ulnar nerve…

Leave a Reply