Introduction
-
The Unhappy Triad, also known as O’Donoghue’s Triad, is a severe and complex knee injury involving damage to three major stabilizing structures of the knee joint.
-
It was first described in the nineteen fifties by Don O’Donoghue, who identified this injury pattern in athletes, particularly those involved in contact sports.
-
The injury classically consists of simultaneous damage to:
-
The anterior cruciate ligament
-
The medial collateral ligament
-
The medial meniscus
-
-
It usually occurs due to a traumatic force applied to the knee, leading to significant instability and functional impairment.
-
A thorough understanding of biomechanics, diagnosis, treatment strategies, and rehabilitation is essential for clinicians, physiotherapists, and sports medicine professionals.
Historical Background
-
Don O’Donoghue was a pioneering orthopaedic surgeon who made significant contributions to the understanding of sports-related knee injuries.
-
In his original observations, he noted that injuries to the anterior cruciate ligament, medial collateral ligament, and medial meniscus frequently occurred together during contact sports.
-
Early diagnosis relied mainly on clinical examination and intraoperative findings due to limited imaging and surgical techniques.
-
Advances in magnetic resonance imaging and arthroscopy later refined the understanding of these injuries.
-
Subsequent research has shown that the lateral meniscus may be injured more frequently than initially thought, leading to reconsideration of the classic triad concept.
Anatomy of the Knee Joint
-
The knee is a synovial hinge joint formed by articulation between:
-
Femur
-
Tibia
-
Patella
-
Key Anatomical Structures
-
Ligaments:
-
Anterior cruciate ligament
-
Posterior cruciate ligament
-
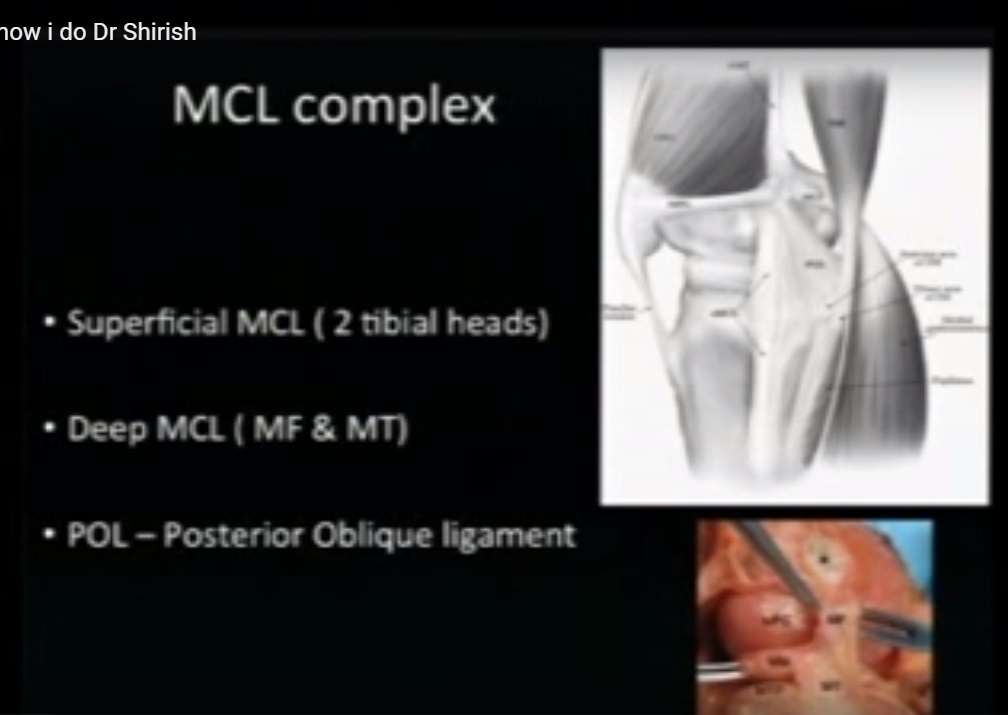
Medial collateral ligament
-
Lateral collateral ligament
-
-
Menisci:
-
Medial meniscus
-
Lateral meniscus
-
-
Articular cartilage:
-
Covers bone surfaces and allows smooth joint motion
-
-
Joint capsule and synovial membrane:
-
Enclose the joint and produce synovial fluid for lubrication
-
Functional Roles
-
The anterior cruciate ligament provides rotational stability and prevents forward translation of the tibia.
-
The medial collateral ligament resists inward valgus stress.
-
The menisci distribute load, absorb shock, and improve joint stability.
Components of the Unhappy Triad
Anterior Cruciate Ligament
-
Primary stabilizer of the knee.
-
Prevents anterior translation of the tibia relative to the femur.
-
Commonly injured through non-contact mechanisms such as pivoting or sudden deceleration.
Medial Collateral Ligament
-
Located on the inner side of the knee.
-
Resists valgus forces.
-
Often injured due to a blow to the lateral aspect of the knee.
Medial Meniscus
-
Provides cushioning and stability.
-
Frequently torn in association with ligament injuries.
Mechanism of Injury
-
Typically results from a blow to the lateral side of the knee with the foot planted and the knee slightly flexed.
-
Valgus stress leads to medial collateral ligament injury.
-
Rotational forces and anterior shear cause rupture of the anterior cruciate ligament.
-
The medial meniscus, being firmly attached to the medial collateral ligament, is subjected to shear and compressive forces, resulting in tearing.
-
Can occur with or without direct contact.
-
Non-contact injuries often involve pivoting with the foot fixed on the ground.
Clinical Presentation
-
Audible or perceived popping sensation at the time of injury.
-
Immediate pain and swelling.
-
Sensation of knee instability or giving way.
-
Rapid swelling due to bleeding within the joint.
Examination Findings
-
Positive Lachman test indicating anterior cruciate ligament injury.
-
Increased valgus laxity suggesting medial collateral ligament damage.
-
Joint line tenderness and mechanical symptoms indicating meniscal injury.
-
Reduced range of motion.
-
Antalgic gait and reluctance to bear weight.
Diagnostic Evaluation
Clinical Assessment
-
Detailed history focusing on injury mechanism.
-
Inspection for swelling, deformity, and instability.
-
Targeted physical tests for ligament and meniscal injuries.
Imaging
-
Radiographs to exclude fractures, particularly tibial plateau fractures.
-
Magnetic resonance imaging as the gold standard for evaluating ligament and meniscal injuries.
-
Ultrasonography may assist in detecting effusion and collateral ligament injuries.
Arthroscopy
-
Used when diagnosis is uncertain or for definitive management.
-
Allows direct visualization and treatment of intra-articular pathology.
Differential Diagnosis
-
Isolated anterior cruciate ligament tear
-
Isolated medial collateral ligament injury
-
Isolated meniscal tear
-
Posterior cruciate ligament injury
-
Patellar dislocation or subluxation
-
Tibial plateau fracture
-
Osteochondral injuries
-
Multiligament knee injuries involving the lateral collateral ligament or posterolateral corner
Injury Grading and Classification
Medial Collateral Ligament Injury
-
Grade One: Mild sprain without instability
-
Grade Two: Partial tear with moderate laxity
-
Grade Three: Complete rupture with significant instability
Anterior Cruciate Ligament Injury
-
Typically complete rupture in the unhappy triad
-
Partial tears are uncommon and difficult to diagnose
Meniscal Injury
-
Vertical, horizontal, bucket-handle, or complex tear patterns
-
Healing potential depends on tear location and vascular supply
Conservative Management
-
Reserved for low-demand individuals or incomplete injuries.
-
Initial treatment includes:
-
Rest
-
Ice application
-
Compression
-
Elevation
-
-
Pain management with non-steroidal anti-inflammatory medications.
-
Knee bracing for stability.
-
Physiotherapy focusing on:
-
Restoration of range of motion
-
Quadriceps and hamstring strengthening
-
Proprioception and neuromuscular control
-
-
Close follow-up for persistent instability.
Indications for Surgical Treatment
-
Complete anterior cruciate ligament rupture in active individuals.
-
Combined ligament and meniscal injuries with instability.
-
Failure of conservative treatment.
-
Large or unstable meniscal tears.
-
Associated cartilage damage.
-
Professional or competitive athletes.
Surgical Techniques
Anterior Cruciate Ligament Reconstruction
-
Performed arthroscopically.
-
Graft options include patellar tendon or hamstring tendon.
-
Accurate tunnel placement and secure fixation are essential.
Meniscal Repair
-
Preferred over meniscectomy to preserve joint function.
-
Techniques include inside-out, outside-in, and all-inside repairs.
-
Best outcomes in well-vascularized peripheral tears.
Medial Collateral Ligament Management
-
Most complete tears heal with non-operative treatment.
-
Surgery indicated for persistent instability or associated multiligament injuries.
Rehabilitation Protocol
Phase One (Zero to Two Weeks)
-
Pain and swelling control
-
Gentle range of motion exercises
-
Use of brace and crutches
Phase Two (Two to Six Weeks)
-
Gradual progression to full weight bearing
-
Closed-chain strengthening exercises
-
Improvement in knee motion
Phase Three (Six to Twelve Weeks)
-
Progressive muscle strengthening
-
Balance and proprioceptive training
Phase Four (Three to Six Months)
-
Advanced functional training
-
Agility and sport-specific drills
Phase Five (Six to Twelve Months)
-
Return to high-intensity activities
-
Based on functional testing and psychological readiness
Prognosis
-
Most patients return to pre-injury activity levels with appropriate treatment.
-
Prognosis depends on:
-
Severity of injury
-
Surgical technique
-
Rehabilitation adherence
-
Patient motivation
-
-
Risk of reinjury remains, particularly in high-level athletes.
-
Long-term risks include chronic instability and osteoarthritis.
Complications
Short-Term
-
Infection
-
Stiffness
-
Hemarthrosis
-
Wound healing issues
Long-Term
-
Graft failure
-
Residual instability
-
Cartilage degeneration
-
Post-traumatic osteoarthritis
-
Psychological fear of reinjury
Advances and Ongoing Research
-
Biological augmentation using platelet-rich plasma and cell-based therapies.
-
Improved graft options and fixation devices.
-
Personalized rehabilitation protocols based on biomechanics and sport-specific demands.
-
Use of wearable technology to monitor rehabilitation progress.
Conclusion
-
The Unhappy Triad represents a severe knee injury requiring a multidisciplinary approach.
-
Early diagnosis, accurate imaging, and individualized treatment are critical for optimal outcomes.
-
Advances in surgical reconstruction and rehabilitation have significantly improved recovery.
-
Injury prevention strategies remain essential in high-risk athletic populations.

Leave a Reply