Courtesy: Prof William Levine, Past President, ASES
Historical Evolution of Shoulder Arthroplasty
Professor Levine outlined six innovation eras.
Era 1: Early Shoulder Arthroplasty (Late 1800s–1950s)
-
Themistocles Gluck (Germany)
-
First shoulder arthroplasty
-
Modular ivory prosthesis
-
Not widely recognized at the time
-
-
Jules Péan (France)
-
First documented shoulder replacement (1893)
-
Two-stage procedure
-
Ultimately failed due to infection
-
-
Early 20th century:
-
Limited options
-
Humeral head resection or arthrodesis for fractures
-
Era 2: Neer Era (1950s–1990s)
-
Dr. Charles Neer
-
Introduced humeral head replacement for fractures
-
Developed Neer I and Neer II systems
-
Transitioned to total shoulder arthroplasty
-
Impact:
-
Disruptive innovation
-
TSA shown superior to hemiarthroplasty in:
-
Patient outcomes
-
Durability
-
Satisfaction
-
Era 3: Grammont Era – Reverse Shoulder Arthroplasty
-
Paul Grammont (1985)
-
Medialized center of rotation
-
Semiconstrained design
-
Increased deltoid lever arm
-
Enabled treatment of pseudoparalytic shoulders
-
Benefits:
-
Allowed treatment of cuff tear arthropathy
-
Reliable stability
Limitations:
-
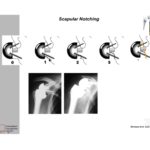
Scapular notching
-
Osteolysis
-
Poor external rotation
-
Humeral bone loss
-
Shoulder contour changes
Era 4: Lateralization Improvements
-
Mark Frankle
-
Lateralized center of rotation
-
Improved rotation
-
Reduced scapular notching
-
Resulted in modern RSA systems.
Era 5: Convertible and Stemless Systems
Convertible Stems
Purpose:
-
Allow conversion from anatomic TSA to RSA without stem removal.
However:
-
Literature shows up to 42–49% of “convertible” stems still require revision.
-
Stem removal increases:
-
Blood loss
-
Surgical time
-
Complication rates
-
True Convertible Concept
-
Stem positioned below osteotomy level
-
Allows easier conversion to reverse
Era 6: Technology Integration
1. Preoperative Planning
-
100% CT-based planning
-
Virtual templating
-
Important in training settings
2. Custom Implants
-
Used for severe deformity or bone loss
-
Patient-specific instrumentation
3. Intraoperative Navigation
-
Real-time execution of surgical plan
-
Improves precision
4. Robotics
-
Highly accurate
-
Clinical superiority not yet proven
-
Workflow integration still evolving
Pyrocarbon Hemiarthroplasty
-
Reduced wear properties
-
Some promising short-term results
Concerns:
-
Glenoid erosion (23%)
-
Implant position changes
-
~8% revision rate at 2 years
Conclusion:
-
Likely similar limitations as traditional hemiarthroplasty
Is Anatomic TSA Obsolete?
Professor Levine argues:
“Do not throw away the anatomic total shoulder.”
Long-Term Strengths of Anatomic TSA
-
Excellent long-term outcomes
-
Superior patient-reported satisfaction compared to RSA
-
Better motion in well-selected patients
Major Concerns
-
Glenoid loosening
-
Subscapularis failure
-
Rotator cuff deterioration
Glenoid Loosening
Large registry data (35,000+ procedures):
-
Glenoid loosening = 26% of failures
-
Rotator cuff insufficiency = 17%
-
Instability and infection also significant
Hybrid Glenoid Design
Modern solution:
-
Cemented peripheral pegs
-
Trabecular metal central peg (bone ingrowth)
Results:
-
1–2% failure rate at 10 years
-
Markedly improved durability
Professor Levine considers hybrid glenoid the current gold standard.
Vitamin E-Enhanced Polyethylene
Benefits:
-
Reduces oxidation
-
Improves wear resistance
-
Maintains mechanical strength
-
Reduced osteolysis
Adopted in modern systems.
Indications: Anatomic vs Reverse
Reverse Shoulder Arthroplasty
Strong Indications:
-
Cuff tear arthropathy
-
Pseudoparalysis
-
Elderly 3- or 4-part proximal humerus fractures
Concerns:
-
Increasing complications
-
Re-revision rate nearly 30%
-
Overall complication rate ~33% in revision RSA
Not benign when it fails.
Anatomic TSA Preferred When:
-
Centered humeral head
-
Intact and functional rotator cuff
-
Adequate glenoid vault
-
Good subscapularis quality
Professor Levine’s current practice:
-
~55–60% anatomic TSA
-
~40–45% reverse
Concerns About Overuse of Reverse
-
Some surgeons perform 100% RSA
-
Trainees may not even see anatomic TSA
-
Potential future epidemic of reverse complications
Comparison made to decline of open Bankart procedures in instability surgery.
Training and Virtual Reality
-
VR training (e.g., Precision OS) can supplement cadaver training
-
Promising educational tool
-
Not yet a full replacement
-
Future vision: AI-driven real-time guidance without CT scans
Key Takeaways
-
Shoulder arthroplasty has evolved through six major innovation eras.
-
Reverse arthroplasty is transformative but not complication-free.
-
Anatomic TSA remains superior in well-selected cuff-intact patients.
-
Hybrid glenoid designs significantly reduce loosening.
-
Vitamin E polyethylene improves implant longevity.
-
Overuse of reverse arthroplasty may create future revision challenges.
-
Young surgeons must maintain expertise in anatomic TSA.
Final Message
Anatomic total shoulder arthroplasty is not extinct.
It remains:
-
A powerful procedure
-
Biomechanically sound
-
Often superior when properly indicated
Careful patient selection and understanding of implant evolution remain essential.




Leave a Reply