Management of Scapho-trapezio-trapezoid Osteoarthritis
Core Review:
- The scaphotrapeziotrapezoid (STT) joint is a common location of degenerative osteoarthritis (OA) in the wrist.
- STT OA may occur in isolation or with concomitant thumb carpometacarpal joint (CMCJ) OA or scapholunate advanced collapse (SLAC) and other wrist OA patterns.
- Nonoperative management strategies include activity modification, bracing, anti-inflammatory medications, occupational therapy, and injections.
- Surgical treatment may be determined by whether the STT OA occurs in isolation or with concomitant thumb CMCJ or SLAC OA and includes STT arthrodesis, distal scaphoid excision with or without interposition or implant arthroplasty, trapeziectomy with proximal trapezoid excision, four-corner fusion in combination with scaphoid/radial column excision, proximal row carpectomy.
PREVALENCE
- OA in the hand and wrist. >75 yrs
- FIRST- thumb carpometacarpal joint (CMCJ) -40 %
- SECOND- radiocarpal joint (secondary to scapholunate advanced collapse [SLAC])- 14%
- scaphotrapeziotrapezoid (STT) joint is the THIRD M.C LOCATION.
- more common in the elderly and in women
- STTOA is commonly associated with other hand and wrist pathologies, including
- Thumb CMCJ And SLAC OA.
Pathophysiology
- traumatic injury to the scaphotrapezial ligamentous complex and membranous portion of the scapholunate interosseous ligament.
Predisposing factors
- atraumatic loosening of STT
- type II lunate morphology
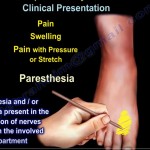
Clinical Presentation
- progressive, aching thumb and radial-sided wrist pain -predominant symptoms.
- pinch and opening a jar are weak and painful.
- Pain exacerbated with with resisted wrist extension and/or radial deviation.
Diagnostic Imaging
- minimum of 3 planes (anteroposterior [AP], lateral, and oblique) to visualize the STT joint and thumb CMCJ thoroughly.
- KAPANDJI AND EATON VIEWS
• FINDINGS- Advanced joint space narrowing, sclerosis, subchondral cyst, osteophyte formation
GRADE OF STT OA as described by White et al.
Posteroanterior radiographs of the wrist demonstrating:
• Stage I OA defined as STT joint space narrowing when compared with adjacent joints of the hand and wrist with or without subchondral sclerosis.
• Stage II OA defined as STT joint space narrowing with subchondral sclerosis compared with adjacent joints of the hand and wrist with or without subchondral cysts and osteophytes.
• Stage III OA defined as complete STT joint narrowing.
The radiographic appearance of STT OA may not be consistent with visual inspection of cartilage intraoperatively.
Nonoperative Treatment
- The cornerstone -activity modification.
- altering or limiting activities and motions that elicit or aggravate symptoms, particularly those who require forceful pinch.
- Short thumb opponens splint.
Pharmacotherapy
- The American College of Rheumatology and Arthritis Foundation Guideline for the Management of OA of the Hand, Hip, and Knee
- STRONGLY RECOMMENDS -oral nonsteroidal anti-inflammatory drug (NSAID)
- conditionally recommended. -Chondroitin sulfate, tramadol, acetaminophen, duloxetine, and topical NSAID medications
- conditionally recommended against- Hyaluronic acid, opioids, colchicine, capsaicin, fish oil, and vitamin D
- strongly recommended against methotrexate, hydroxychloroquine, bisphosphonates, and glucosamine.
Intra-articular injection therapy
- Corticosteroids may be combined with lidocaine
- The use of PRP injections for STT OA is still controversial
Operative Treatment
- Complex and controversial, Failed conservative management
- STT arthrodesis,
- distal scaphoid excision with or without interposition or implant arthroplasty,
- trapeziectomy with proximal trapezoid excision,
- four-corner fusion (4CF) in combination with scaphoid/radial column excision
- proximal row carpectomy (PRC)
STT Arthrodesis
- Arthrodesis of the STT joint may be accomplished using multiple constructs including
smooth Kirschner wires,circular plate, and screw constructs - overall postoperative range of motion was 70% to 80%
- strength was 69% to 89% of the unaffected side
- 88% returning to previous employment.
- complication rate of 13.4% and nonunion in 4%..
Distal Scaphoid Resection with or without Interposition
- technically simpler procedure
- approached open, arthroscopically, volarly, or dorsally
- relieves pain by removing the pathologic articulation
- interposition done with usually palmaris longus tendon.
Distal Scaphoid Resection and Implant Arthroplasty
- Originally, the Swanson silicone trapezium implant was used.
- pyrocarbon implants – revitalized the idea of implant arthroplasty.
- primarily composed of pyrolytic carbon (a form of carbon) coating a graphite substrate
Trapeziectomy and Proximal Trapezoid Excision
- Trapeziectomy with or without ligament reconstruction and interposition (LRTI) is commonly performed for advanced thumb CMCJ OA.
- When performed in conjunction with proximal trapezoid excision, the arthritic STT joint is removed entirely. This procedure is often used in the treatment of STTOA
- FCR interposition arthroplasty may be used in conjunction with trapeziectomy and proximal trapezoid excision – concomitant STT and thumb CMCJ OA.
Suspensionplasty After Trapeziectomy
- Suspensionplasty -technique to reduce the risk of metacarpal subsidence after trapeziectomy.
• using native ligaments such as the abductor pollicis longus,
• surgical devices such as suture or suture buttons,
• to preserve metacarpal height & maintain the relative alignment of the first and second metacarpals.
Concomitant Thumb CMCJ, STT, and Scaphoid Lunate Advanced Collapse OA
• uncommon
• Two surgical techniques
• -radial column excision with four corner fusion
PROXIMAL ROW CARPECTOMY
Radial Column Excision and four corner fusion
- Radial column excision -excision of both the trapezium and scaphoid.
- 4CF was first popularized by Watson and Ballet to treat radiocarpal OA
-scaphoid resection and arthrodesis between the lunate, capitate, hamate, and triquetrum with the use of Kirschner wires.
• Instrumentation including a circular dorsal plate and screws, compression screws, or staples is often used.
Proximal Row Carpectomy
• PRC is a motion-preserving technique in the surgical management of SLAC
• may be combined with trapeziectomy for those with concurrent thumb CMCJ, STT, and SLAC OA.
• flexion and extension-comparable, grip strength was lower
Total Wrist Denervation for STT OA and Concomitant Pathologies
• Promising outcomes-selective denervation for pure symptomatic pain alleviation
• Can be opted in elderly(PIN & AIN)
low morbidity rates, early return to work, preservation or improvement of functional mobility, and high patient satisfaction rates.

Thiank you