Courtesy: Prof Nabil Ebraheim, University of Toledo, Ohio, USA
Heel Pain: Causes, Diagnosis, and Management
Overview
Heel pain is a very common musculoskeletal complaint with multiple potential causes.
Many of these conditions occur in closely related anatomical regions, leading to:
- Overlapping symptoms
- Diagnostic difficulty
Accurate diagnosis is essential for appropriate treatment and optimal outcomes
Common Causes of Heel Pain
Major Causes
- Plantar fasciitis (most common)
- Baxter nerve entrapment (inferior calcaneal nerve)
- Heel fat pad atrophy
- Achilles tendinitis
- Haglund deformity
- Calcaneal stress fracture
- Tarsal tunnel syndrome
- Lumbosacral radiculopathy
Diagnostic Challenge
- Pain locations overlap around the heel
- Clinical differentiation may be difficult
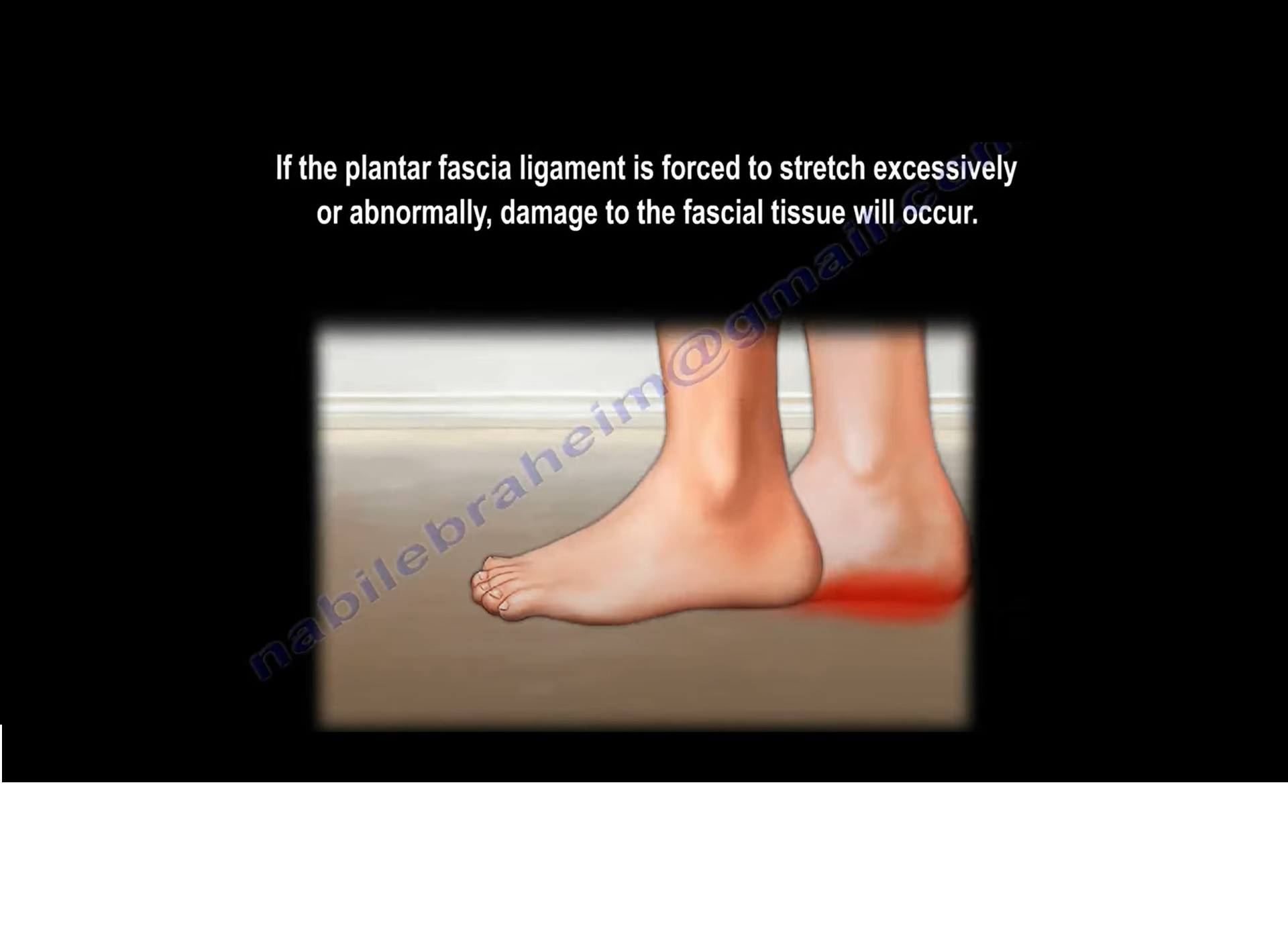
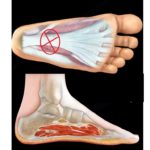
Plantar Fasciitis
Definition
Inflammation or degeneration of the plantar fascia, a thick fibrous band supporting the foot arch.
Pathophysiology
- Repetitive microtrauma
- Fascia thickening and irritation
Clinical Features
- Severe morning start-up pain
- Pain improves initially with walking
- Worsens with:
- Prolonged standing
- Walking
- Exercise
Examination
- Point tenderness at plantar medial heel
- Negative Tinel sign (helps exclude nerve entrapment)
Imaging
- X-ray may show heel spur
- Spur is associated but not causative
Associated Factors
- Tight Achilles tendon
Treatment
- Night splints
- Physiotherapy
- Heel cushions / silicone inserts
- Achilles stretching
- Corticosteroid injections
Baxter Nerve Entrapment
Anatomy
- First branch of the lateral plantar nerve
- Supplies abductor digiti minimi
Course
- Between:
- Abductor hallucis
- Quadratus plantae
- Turns laterally beneath calcaneus
Clinical Importance
- Accounts for ~20% of chronic heel pain
- Frequently misdiagnosed as plantar fasciitis
Symptoms
- Medial plantar heel pain
- Common in runners
Heel Fat Pad Atrophy
Pathophysiology
- Thinning of heel fat pad
- Loss of shock absorption
Risk Factors
- Elderly
- Repeated steroid injections
Clinical Features
- Deep central heel pain
- Worse when barefoot
- Better when walking on toes
Examination
- Central heel tenderness
Treatment
- Footwear modification
- Heel padding
- Shock-absorbing insoles
Achilles Tendinitis
Features
- Posterior heel pain
- Tendon thickening
- Swelling
Treatment
- Immobilization
- Eccentric strengthening
- Physiotherapy
Haglund Deformity
Definition
Bony prominence of the posterosuperior calcaneus
Associations
- Retrocalcaneal bursitis
- Insertional Achilles tendinopathy
Conservative Treatment
- Physiotherapy
- Anti-inflammatory medication
Injection Caution
- Avoid injecting into Achilles tendon
- Only inject around the tendon
Surgical Indications
- Persistent symptoms >6 months
Surgical Options
- Excision of bony prominence
- Removal of calcifications
Advanced Cases
If >50% Achilles tendon involved:
- Tendon reconstruction required
Options
- Suture anchors
- Flexor hallucis longus (FHL) tendon transfer
Calcaneal Stress Fracture
Cause
- Repetitive loading / overuse
Symptoms
- Severe weight-bearing pain
- Persistent throughout the day
Examination
- Positive calcaneal squeeze test
Diagnosis
- X-ray may be normal initially
- MRI is more sensitive
Treatment
- Immobilization:
- Boot or cast
Tarsal Tunnel Syndrome
Definition
Compression of the posterior tibial nerve in the tarsal tunnel
Symptoms
- Tingling or numbness in plantar foot
- Worsens with activity
- Night pain
Causes
- Ganglion cyst
- Space-occupying lesions
Diagnosis
- MRI to identify compressive cause
Treatment
- Surgical decompression
- Excision of lesion if present
Lumbosacral Radiculopathy
Cause
- Commonly due to L5–S1 disc herniation
Symptoms
- Pain along lateral foot
- Sensory changes
Clinical Importance
- May mimic heel pathology
Diagnostic Approach
Essential Components
- Detailed history
- Focused physical examination
- Imaging when necessary
Key Principle
Differentiate between:
- Mechanical causes
- Neurological causes
- Soft tissue vs bony pathology
Key Clinical Points
- Heel pain has multiple overlapping causes
- Plantar fasciitis is the most common but not the only diagnosis
- Misdiagnosis is common without careful evaluation
Take-Home Message
- Always consider a broad differential diagnosis
- Use a systematic clinical approach
- Accurate diagnosis leads to:
- Targeted treatment
- Better patient outcomes

Leave a Reply