Courtesy: David Bennett, MD, is a board certified orthopedic and spine surgeon at Phoenix Children’s Hospital
Assistant Professor, University of Arizona
Pediatric Orthopaedic Infections
Pediatric orthopaedic infections commonly include:
-
Septic arthritis
-
Osteomyelitis
-
Spine infections
-
Pyomyositis
1. Pediatric Septic Arthritis
Overview
-
Septic arthritis is the most common pediatric orthopaedic infection.
-
It most frequently presents between 1 month and 5 years of age.
-
Approximately 50 percent of cases occur in children younger than 2 years.
-
About 94 percent of cases involve a single joint.
-
The hip is the most commonly affected joint in children.
Etiology
Common causative organisms vary by age and clinical context:
-
Staphylococcus aureus: common at all ages
-
Haemophilus influenzae: children aged 6 months to 5 years who are unvaccinated
-
Neisseria gonorrhoeae: children older than 10 years
-
Gram-negative bacilli: immune deficiency, urinary or gastrointestinal procedures, penetrating trauma, renal failure, chronic joint disease, diabetes
-
Staphylococcus aureus and Pseudomonas: puncture wounds
-
Streptococcus pneumoniae: pneumonia, meningitis, upper respiratory tract infections
-
Listeria monocytogenes: immune deficiency
-
Atypical mycobacteria: chronic infections
-
Group B streptococcus: maternal transmission in neonates
Pathogenesis
-
Hematogenous spread (most common)
-
Spread from adjacent tissues
-
Direct inoculation following aspiration or arthrotomy
Risk factors include:
-
Rheumatologic diseases
-
Structural joint abnormalities
-
Steroid use
-
Diabetes mellitus
-
Immune deficiency
-
Hematologic disorders
-
Trauma
-
Systemic infections
Hematogenous Spread
Common sources include:
-
Otitis media
-
Sinusitis
-
Pneumonia
-
Dental infections
-
Skin inoculation
In neonates, metaphyseal and epiphyseal blood supplies communicate, allowing infection to spread into the epiphysis and potentially cause osteonecrosis. After development of the secondary ossification center, the growth plate acts as a barrier, although metaphyseal infections may still decompress into the joint.
Joints at High Risk (S.H.A.E.)
-
Shoulder
-
Hip
-
Ankle
-
Elbow
These joints have intracapsular physes, predisposing them to septic arthritis.
Clinical Presentation
Key clinical features include:
-
Fever
-
Acute joint pain
-
Swelling and warmth
-
Joint effusion
-
Severe restriction of motion
-
Pain with minimal movement
-
Limp or inability to bear weight
Diagnostic Approach
A systematic approach is essential:
History
-
Recent infections
-
Immunization status
-
Nutritional status
-
Trauma
-
Antibiotic exposure
-
Symptom onset and progression
Physical Examination
-
Joint position at rest
-
Pain with motion
-
Log roll test
-
Gait assessment
-
Swelling, tenderness, warmth
Investigations
Laboratory Tests
Complete Blood Count
-
White cell count above 12,000 may be present
-
Elevated neutrophil percentage
-
Only 25 to 35 percent have elevated counts at presentation
-
Helps exclude leukemia
Erythrocyte Sedimentation Rate
-
Peaks in 3 to 5 days
-
Returns to normal within 3 weeks
-
Less reliable than C-reactive protein
C-Reactive Protein
-
Most sensitive marker
-
Rises within 6 hours
-
Peaks at 24 to 50 hours
-
Normalizes within 7 to 11 days
-
Useful for monitoring treatment response
-
Rising levels suggest concurrent osteomyelitis
-
A normal value does not completely exclude septic arthritis
Imaging
-
Radiographs as the first investigation
-
Ultrasound to detect joint effusion
-
Magnetic resonance imaging with and without contrast if indicated
-
Bone scan when diagnosis remains unclear
Joint Aspiration (Gold Standard)
-
Performed at bedside, in the operating room, or by interventional radiology
-
Fluid analysis includes:
-
Appearance
-
Cell count
-
Protein and glucose
-
Gram stain and culture
-
-
White cell count above 50,000 with neutrophil predominance is suggestive
-
Cultures may be negative in 18 to 70 percent of cases
Management
Antibiotic Therapy
-
Based on culture results
-
Empiric therapy if cultures are negative
-
Typical duration is 4 to 6 weeks
-
Infectious disease consultation recommended
Surgical Management
-
Drainage after cultures are obtained
-
Antibiotics withheld until cultures unless patient is septic
-
Drain placement
-
Repeat irrigation based on clinical and laboratory response
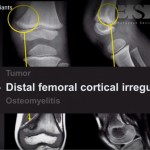
2. Pediatric Osteomyelitis
Classification
-
Acute
-
Subacute
-
Chronic
-
Chronic recurrent multifocal osteomyelitis
Clinical Features
-
Less severe symptoms than septic arthritis
-
Pain, tenderness, warmth
-
Mild to moderate swelling
-
Patients may still be able to walk
Laboratory Findings
-
White cell count elevated in 25 to 50 percent
-
Left shift in 40 to 60 percent
-
Erythrocyte sedimentation rate elevated in 90 percent
-
C-reactive protein elevated in 98 percent
-
Blood cultures positive in 30 to 50 percent
Imaging
-
Radiographs may be normal for 10 to 14 days
-
Bone changes visible only after 30 to 50 percent density loss
-
Magnetic resonance imaging is 98 percent sensitive
-
Detects abscess, pyomyositis, deep vein thrombosis, septic arthritis
Acute Hematogenous Osteomyelitis
-
Most commonly metaphyseal
-
Femur most frequent site
-
Long bones involved in 75 percent
Management
-
Broad-spectrum empiric antibiotics
-
Targeted therapy once cultures available
-
Surgical drainage if abscess or failure of antibiotics
-
Early treatment reduces chronic conversion
Complications
-
Chronic osteomyelitis
-
Avascular necrosis
-
Growth arrest
-
Deep vein thrombosis
-
Pulmonary embolism
-
Sepsis
-
Pathologic fracture
Subacute Osteomyelitis
-
Insidious onset
-
Mild symptoms
-
Often normal laboratory values
-
Mimics bone tumors
-
Magnetic resonance imaging with contrast is essential
-
Cultures positive in 29 to 61 percent
Chronic Osteomyelitis
-
Often follows acute infection
-
Tibia is most common site
-
Sequestrum formation with involucrum
-
Requires prolonged antibiotics and surgery
-
Antibiotic-loaded cement beads may be used
3. Pediatric Spine Infections
Overview
-
Accounts for 1 to 2 percent of pediatric osteomyelitis
-
Discitis common under 7.5 years
-
Vertebral body osteomyelitis managed similarly
Clinical and Diagnostic Features
-
Lumbar spine most commonly involved
-
Cultures positive in 30 to 50 percent
-
Magnetic resonance imaging sensitivity 96 percent
-
Blood cultures guide therapy
-
Antibiotics for 6 weeks to 6 months
-
Brace may help pain
-
Long-term disc space narrowing and fusion possible
Necrotizing Fasciitis
Key Points
-
High mortality rate
-
Early diagnosis is critical
-
Only proven mortality-reducing factor is early surgical debridement
-
Severe pain, swelling, bullae, skin necrosis, crepitus
-
Requires emergency surgery and intravenous antibiotics
4. Pyomyositis
Overview
-
Often preceded by trauma
-
Typically involves a single muscle group
-
Quadriceps most commonly affected
-
Spread is usually hematogenous
Diagnosis
-
Magnetic resonance imaging with contrast is diagnostic
-
Rim thickness predicts response to antibiotics
-
Guides surgical planning
Treatment
-
Empiric antibiotics for 4 to 6 weeks
-
Image-guided drainage when possible
-
Surgery for loculated abscesses or systemic toxicity
Complications
-
Can be aggressive, especially streptococcal infections
-
Mortality can be high in severe cases
Septic Bursitis
Clinical Features
-
Swelling, erythema, tenderness
-
Pain with motion but preserved range
-
Most commonly caused by Staphylococcus aureus
Management
-
Aspiration if diagnosis uncertain
-
Antibiotic therapy based on organism
-
Incision and drainage when indicated


Leave a Reply