Courtesy: Dr Shivshankar Challa, MS, MRCS, Mch
Introduction: Overview of Alkaptonuria
-
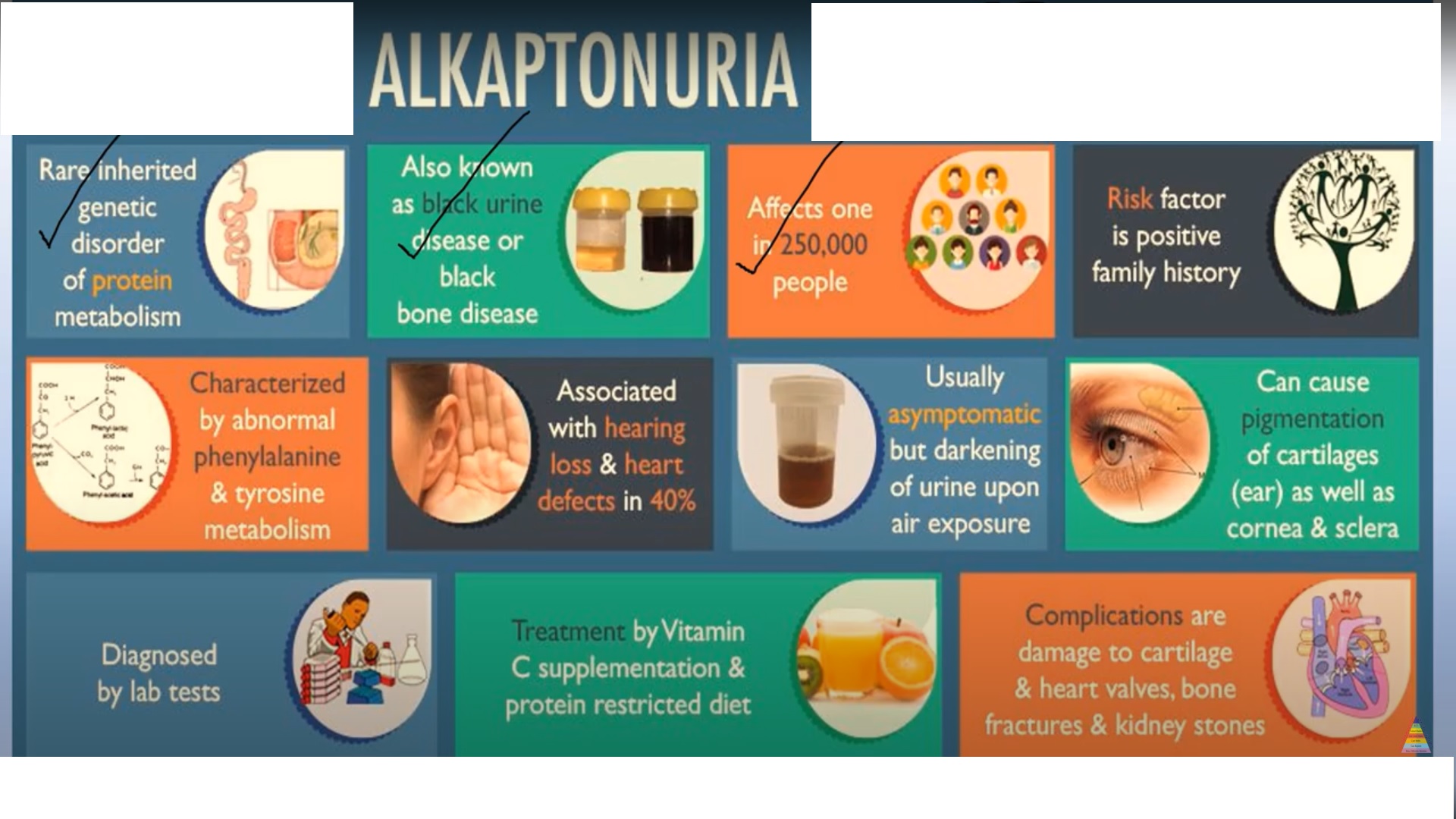
Alkaptonuria is an extremely rare autosomal recessive metabolic disorder.
-
It is caused by deficiency of the enzyme homogentisic acid dioxygenase.
-
The condition affects approximately one in two hundred and fifty thousand to one in one million live births.
-
Under normal metabolism, homogentisic acid is converted to maleylacetoacetic acid.
-
In alkaptonuria, this metabolic pathway is disrupted, leading to:
-
Accumulation of homogentisic acid
-
Deposition of its oxidized product, benzoquinone acetic acid, in collagen-rich tissues
-
-
Excess homogentisic acid is excreted in urine, which:
-
Darkens on standing
-
Darkens on alkalinization
-
-
This urinary discoloration gives the disease its name.
Classic Triad of Alkaptonuria
-
Homogentisic aciduria
-
Presence of homogentisic acid in urine
-
-
Ochronosis
-
Bluish-black pigmentation of connective tissues
-
-
Ochronotic arthropathy
-
Progressive degenerative joint disease
-
Ochronosis
-
Refers to deposition of pigmented metabolic by-products in connective tissues.
-
Pigment appears yellow or ochre microscopically.
-
Most commonly affects:
-
Hyaline cartilage
-
-
Results in:
-
Cartilage discoloration
-
Structural damage
-
-
Also causes pigmentation of:
-
Eyes
-
Skin
-
Systemic Manifestations of Alkaptonuria
Cardiovascular System
-
Coronary artery calcification
-
Valvular calcification
-
Possible development of aortic stenosis
Respiratory System
-
Stiffening of costal cartilage
-
Reduced chest expansion
-
Exertional breathlessness
Genitourinary System
-
Formation of:
-
Renal stones
-
Urethral stones
-
Prostatic stones
-
Skeletal System
-
Osteopenia
-
Osteoporosis
-
Increased fracture risk
Tendons
-
Ochronotic tendinopathy commonly affects:
-
Achilles tendon
-
Patellar tendon
-
-
May lead to:
-
Enthesopathy
-
Spontaneous tendon rupture
-
Ochronotic Arthropathy
General Characteristics
-
Most common complication of alkaptonuria.
-
Usually asymptomatic until the fourth decade of life.
-
Progression correlates with declining renal clearance of homogentisic acid.
Clinical Features
-
Progressive joint pain
-
Swelling
-
Stiffness
-
Restricted range of motion
-
Functional limitation
-
Reduced quality of life
Commonly Affected Joints
-
Spine:
-
Cervical region
-
Thoracic region
-
Lumbosacral region
-
-
Peripheral joints:
-
Knee is most frequently affected
-
Historical Perspective of Alkaptonuria
-
Fifteen hundred years before the common era
-
Evidence of ochronosis identified in the Egyptian mummy Harwa
-
-
Fifteen eighty-four
-
Scribonius described a child passing black urine
-
-
Eighteen fifty-nine
-
Boedeker coined the term “alcapton” for a reducing urinary substance
-
-
Eighteen sixty-six
-
Rudolf Virchow introduced the term “ochronosis”
-
-
Eighteen ninety-one
-
Wolkow and Baumann identified homogentisic acid
-
-
Nineteen hundred two
-
Albrecht recognized alkaptonuria and ochronosis as manifestations of the same disease
-
Sir Archibald Garrod identified the hereditary nature
-
-
Nineteen hundred eight
-
Garrod described alkaptonuria as the first inborn error of metabolism
-
-
Nineteen hundred nine
-
Neubauer mapped the tyrosine degradation pathway
-
-
Later research confirmed deficiency of homogentisic acid oxidase as the underlying defect.
Etiopathology of Ochronotic Arthropathy
Impaired Collagen Cross-Linking
-
Benzoquinone acetic acid inhibits lysine hydroxylase.
-
Results in reduced collagen cross-linking.
-
Produces weak connective tissue susceptible to mechanical stress.
-
Leads to cartilage fragmentation.
Synovial Reactions
-
Cartilage fragments adhere to synovium, causing:
-
Inflammation
-
Fibrosis
-
Loose body formation
-
Secondary chondromatosis
-
Altered Cartilage Mechanics
-
Pigmented cartilage becomes:
-
Brittle
-
Less elastic
-
Poorly resistant to mechanical loading
-
Oxidative Stress
-
Oxidation of homogentisic acid generates free oxygen radicals.
-
Leads to:
-
Inflammation
-
Degeneration
-
Amyloid deposition
-
Cellular Effects
-
Oxidative stress impairs osteoblast function.
-
Results in:
-
Autophagy dysfunction
-
Chondrocyte death
-
Bone Resorption
-
Pigment deposition stimulates osteoclastic activity.
-
Causes loss of subchondral bone plate.
Impaired Bone Mineralization
-
Pigment interferes with osteoid mineralization.
-
Results in:
-
Reduced bone mineral density
-
Increased fragility fracture risk
-
Clinical Presentation of Ochronotic Arthropathy
General Pattern
-
Predominantly affects:
-
Spine
-
Large weight-bearing joints
-
-
Small joints are usually spared.
-
Sacroiliac joints are typically unaffected.
-
Absence of:
-
Bamboo spine
-
Annular ossification
-
Syndesmophytes
-
Spinal Involvement
Clinical Features
-
Chronic back pain
-
Spinal stiffness
-
Loss of lumbar lordosis
-
Increased thoracic kyphosis
Severity
-
More severe disease in individuals positive for human leukocyte antigen B-twenty seven.
Radiological Findings
-
Intervertebral disc degeneration
-
Multilevel disc calcification
-
Vacuum phenomenon
-
Possible progression to spinal stenosis with myelopathy
Peripheral Joint Involvement
-
Occurs years after spinal symptoms.
-
Knee is the most commonly involved joint, affecting up to sixty-four percent of patients.
-
Upper limb involvement is rare.
Radiological Features
-
Severe degenerative changes
-
Joint space narrowing
-
Subchondral sclerosis
-
Minimal or absent osteophyte formation
Synovial Fluid Findings
-
Presence of floating black particles
-
Known as the “ground pepper sign”
Rare Associated Conditions
-
Rheumatoid arthritis
-
Ankylosing spondylitis
-
Chondrocalcinosis
Treatment of Alkaptonuria and Ochronotic Arthropathy
General Principles
-
No definitive cure exists.
-
Treatment focuses on:
-
Reducing homogentisic acid levels
-
Symptom control
-
Prevention of complications
-
Conservative Management
Dietary Protein Restriction
-
Reduces homogentisic acid excretion.
-
May improve bone metabolism.
-
Difficult to maintain long term.
Ascorbic Acid Supplementation
-
May reduce oxidation of homogentisic acid.
-
Supports collagen health.
Nitisinone Therapy
-
First disease-modifying therapy approved for alkaptonuria.
-
Approved in Europe in two thousand twenty.
-
Previously approved for hereditary tyrosinemia type one.
Mechanism of Action
-
Inhibits four-hydroxyphenylpyruvate dioxygenase.
-
Reduces production of homogentisic acid.
Clinical Trial Evidence
-
Significant reduction in urinary homogentisic acid levels.
-
Improvement in clinical symptoms and biochemical markers.
-
Limited effect on preventing secondary amyloidosis.
Symptomatic and Supportive Care
-
Physiotherapy to preserve joint mobility.
-
Pain control using non-steroidal anti-inflammatory drugs.
-
No effect on disease progression.
Surgical Management
-
Indicated in end-stage ochronotic arthropathy.
-
Total joint replacement is the most effective option.
-
Most commonly performed for:
-
Hip joints
-
Knee joints
-
Case Summary: Middle-Aged Female with Polyarticular Ochronotic Arthropathy
Clinical Timeline
-
Two thousand sixteen (Age fifty-three)
-
Bilateral anatomic total shoulder replacement
-
-
Two thousand twenty (Age fifty-seven)
-
Severe right hip pain and weight-bearing difficulty
-
Magnetic resonance imaging showed:
-
Osteonecrosis of femoral head
-
Advanced hip arthritis
-
-
Cementless right total hip replacement performed
-
Intraoperative Findings
-
Black discoloration of:
-
Joint capsule
-
Femoral head
-
Synovium
-
-
Complete cartilage separation
-
Diagnosis confirmed as ochronotic arthropathy
Postoperative Complication
-
Six weeks later:
-
Severe left hip pain
-
Rapid cartilage destruction
-
-
Treated with cementless left total hip replacement.
-
Similar intraoperative findings noted.
Postoperative Recovery
-
Mobilized pain-free with crutches on first postoperative day.
-
Intensive physiotherapy and gait training.
-
Walking aids discontinued within three weeks.
Outcome at Two-Year Follow-Up
-
No hip pain
-
Full range of motion
-
Independent in daily activities
-
No implant loosening or subsidence
-
Persistent back pain due to advanced spinal degeneration
Summary of Arthroplasty Outcomes in Ochronotic Arthropathy
-
Multiple published reports demonstrate:
-
Excellent short- and long-term outcomes
-
Successful hip, knee, and shoulder replacements
-
-
Cementless arthroplasty shows:
-
Good implant stability
-
No increased complication rate
-
-
Surgical considerations:
-
Total synovectomy is recommended
-
Preservation of joint capsule improves stability
-
Final Conclusion
-
Alkaptonuric ochronosis is an ultra-rare and disabling metabolic disorder.
-
It leads to progressive polyarticular joint destruction.
-
Affects relatively young individuals.
-
Cementless, bone-preserving total joint replacement:
-
Provides reliable pain relief
-
Restores function
-
Offers excellent long-term outcomes
-
-
Total joint replacement remains the most effective treatment for end-stage ochronotic arthropathy.


Leave a Reply