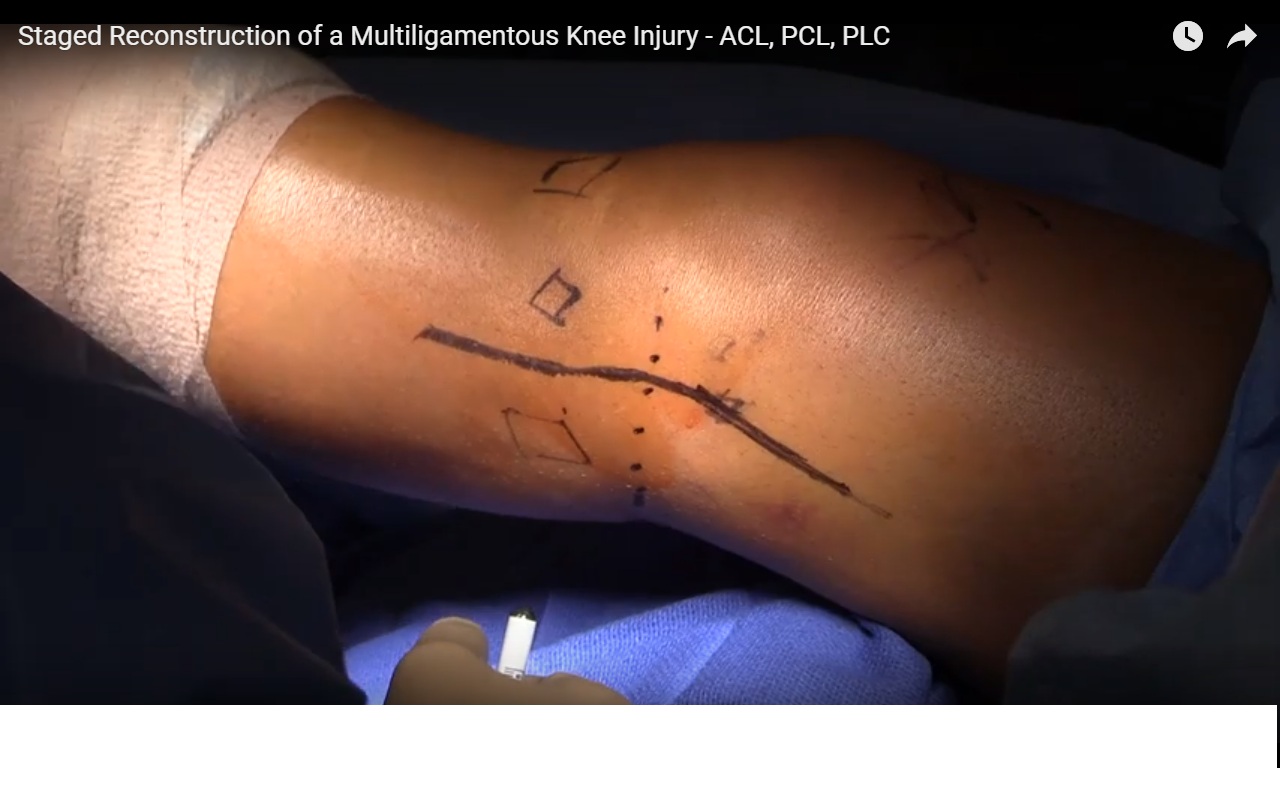
Courtesy: Dr Brett Fritsch, Ashok Shyam, Ortho TV
Management of Multi-Ligament Knee Injuries
Definition
-
A multi-ligament knee injury involves complete disruption of at least two of the four major ligament complexes of the knee.
-
In cases of knee dislocation:
-
Classification is based on the position of the tibia relative to the femur.
-
-
If the dislocation has spontaneously reduced:
-
Classification is based on the direction of the major instability.
-
Nature of the Injury
-
Multi-ligament knee injuries represent a heterogeneous group of injuries.
-
There is no single consistent injury pattern.
-
The variability in ligament combinations and injury mechanisms makes:
-
Clinical research difficult
-
Treatment protocols variable
-
Functional Outcome Expectations
Patients should be counseled realistically about recovery.
Key observations from clinical follow-up studies include:
-
Complete restoration of a normal knee is uncommon.
-
Good outcomes are usually achieved in:
-
Pain relief
-
Activities of daily living
-
-
Limitations often persist in:
-
High-level sports
-
Quality of life measures
-
Activity Levels
-
Many patients lose one Tegner activity level after injury.
Gait Characteristics After Treatment
Patients often demonstrate subtle gait changes:
-
Slightly slower walking speed
-
Shorter step length
-
Increased time spent in stance phase
-
Increased time spent in double-stance phase
These findings suggest persistent caution during weight-bearing activities.
Principles of Management
The approach follows a stepwise improvement strategy similar to the concept of continuous improvement.
Key priorities include:
-
Correct management priorities
-
Accurate diagnosis
-
Appropriate timing of surgery
-
Correct surgical reconstruction
Acute Versus Chronic Presentation
Acute Injuries
-
Often occur in the setting of high-energy trauma.
-
The patient may have multiple injuries.
Management priorities:
-
Stabilize the patient
-
Evaluate and protect the limb
-
Treat the knee injury
Chronic Injuries
-
The patient is medically stable.
-
Focus shifts toward:
-
Identifying the exact instability pattern
-
Planning reconstructive surgery
-
Mechanism of Injury
Most multi-ligament knee injuries result from high-energy trauma.
Common causes include:
-
Road traffic accidents – more than half of cases
-
Sports injuries – approximately one quarter
-
Contact injuries – about two thirds of sports-related cases
Associated Injuries
Multi-ligament knee injuries are frequently associated with other traumatic conditions.
Systemic Injuries
These may include:
-
Thoracic injuries
-
Abdominal trauma
-
Spine injuries
-
Head injuries
-
Long bone fractures
Local Knee Injuries
Common associated injuries include:
-
Soft tissue damage
-
Meniscal tears
-
Tibial plateau fractures
-
Nerve injuries
-
Vascular injuries
Initial Trauma Management
Management follows standard trauma protocols.
Steps include:
-
Primary trauma assessment
-
Immediate vascular examination
-
Neurological examination
-
Reduction of the knee dislocation
-
Stabilization of the joint
Reassessment of vascular and neurological status must be performed after reduction.
Vascular Assessment
Knee dislocations can threaten limb viability.
Reported Incidence
-
Vascular injury occurs in up to fifteen percent of cases in some reports.
Assessment Methods
Common diagnostic methods include:
-
Clinical examination
-
Doppler ultrasound
-
Ankle-brachial index measurement
-
Computed tomography angiography
-
Conventional angiography
Selective Angiography Strategy
A selective imaging approach is commonly used.
Management Algorithm
-
Reduce the knee dislocation.
-
Assess distal perfusion.
If the limb is ischemic
-
Immediate surgical exploration
-
On-table angiography if required
If perfusion is adequate
-
Assess pulse symmetry.
If pulses are asymmetric:
-
Perform computed tomography angiography.
If pulses are symmetric:
-
Measure ankle-brachial index.
Interpretation of Ankle-Brachial Index
-
Index greater than 0.9 ? observation for twenty-four hours
-
Index less than 0.9 ? computed tomography angiography
Neurological Assessment
Neurological examination should be performed:
-
Before reduction
-
After reduction
Structures Assessed
Common Peroneal Nerve
Evaluate:
-
Ankle dorsiflexion strength
-
Foot eversion strength
-
Dorsal foot sensation
Tibial Nerve
Evaluate:
-
Plantar flexion strength
-
Plantar foot sensation
Incidence of Nerve Injury
-
Approximately one third of patients may have nerve injuries in some reports.
Common peroneal nerve injury is particularly associated with posterolateral corner injuries.
Observations
-
Posterolateral corner injuries increase nerve injury risk.
-
Neuropraxia is more common than complete nerve disruption.
However, nerve injury is associated with poorer functional outcomes.
Management of Nerve Injuries
A simple approach can be used:
-
Intact nerve ? decompression and observation
-
Transected nerve ? primary repair if possible
-
Irreparable injury ? tendon transfer may be required
Reduction and Stabilization
Reduction Technique
-
Usually achieved using gentle longitudinal traction and manipulation.
Most dislocations reduce easily unless:
-
Soft tissue interposition is present.
Stabilization Options
After reduction, the knee should be stabilized using the least restrictive method that maintains joint stability.
Common options include:
-
Hinged knee braces
-
Posterior splints
-
Plaster back-slabs
-
External fixation in severe instability
Indications for External Fixation
External fixation may be required in:
-
Open knee dislocations
-
Associated vascular repairs
-
Gross instability not controlled with bracing
Diagnostic Evaluation
Accurate diagnosis requires a combination of:
-
Clinical examination
-
Imaging studies
Clinical Examination
Central Reference Structure
The posterior cruciate ligament is considered the central reference point of the knee.
All ligament assessments should be interpreted relative to:
-
The medial tibiofemoral step-off.
Ligament-Specific Tests
Anterior Cruciate Ligament
-
Lachman test
Medial Collateral Ligament
-
Valgus stress test at zero and thirty degrees
Posterolateral Corner
Multiple tests may be used, including:
-
Varus stress testing
-
External rotation recurvatum test
-
Dial test
-
Posterior drawer test
-
Reverse pivot shift test
Some of these tests are more useful in chronic injuries.
Imaging
Radiographs
Radiographs help to:
-
Identify fractures
-
Confirm reduction
-
Provide clues to ligament injury patterns
Radiographs should be repeated within twenty-four hours to detect secondary subluxation, particularly with tibial plateau fractures.
Magnetic Resonance Imaging
Magnetic resonance imaging is the primary diagnostic imaging tool.
It provides information about:
-
Ligament disruptions
-
Injury locations
-
Associated meniscal injuries
-
Articular cartilage damage
Computed Tomography
Computed tomography is used mainly for:
-
Complex fractures
-
Vascular imaging when angiography is required
Stress Radiographs
Stress radiographs are more useful in chronic instability.
Interpretation guidelines include:
-
Two millimetres of side-to-side opening suggests isolated lateral collateral ligament injury
-
More than four millimetres suggests more severe ligament injury
These studies are technically demanding and should ideally be performed by the surgeon.
Surgical Treatment Principles
Evidence generally supports operative treatment.
Key observations from available studies:
-
Surgical treatment performs better than nonoperative treatment.
-
Ligament reconstruction performs better than simple repair.
-
Early surgery generally produces better outcomes than delayed surgery.
Optimal Timing of Surgery
The ideal surgical window is usually within two to three weeks after injury.
Advantages of This Timing
-
Capsular healing reduces fluid extravasation during arthroscopy.
-
Tissue planes are still identifiable.
-
Repairable structures remain accessible.
Operating too early may cause excessive fluid leakage during arthroscopy.
Operating too late makes anatomical dissection more difficult.
Ligament Reconstruction Strategy
Most surgeons reconstruct:
-
Anterior cruciate ligament
-
Posterior cruciate ligament
-
Posterolateral corner
Posterolateral Corner Injuries
Evidence suggests reconstruction is more reliable than isolated repair.
Reported outcomes:
-
Reconstruction success rates around ninety percent
-
Repair success rates significantly lower
Indications for Repair
Repair may be appropriate when:
-
A large avulsion fragment is present
-
The ligament is attached to a repairable bone fragment
Otherwise, reconstruction is usually preferred.
Chronic Instability and Alignment
In chronic injuries, limb alignment must be evaluated carefully.
Varus malalignment increases stress on ligament reconstructions.
Role of Osteotomy
High tibial osteotomy may:
-
Improve knee stability
-
Improve outcomes of ligament reconstruction
-
Reduce failure rates
In some cases, osteotomy alone can significantly improve stability.
Graft Selection
Graft choice depends on:
-
Number of ligaments being reconstructed
-
Graft length and diameter requirements
-
Availability of graft tissue
-
Surgeon experience
-
Cost and accessibility
Autograft Options
Common options include:
-
Hamstring tendons
-
Quadriceps tendon
-
Patellar tendon
Autografts generally demonstrate good long-term outcomes.
Allograft Options
Allografts may be useful when:
-
Multiple ligaments require reconstruction
-
Autograft tissue is insufficient
Non-irradiated grafts are preferred.
Reconstruction of Individual Ligaments
Anterior Cruciate Ligament
Common technique:
-
Hamstring autograft
-
Anatomical tunnel placement
-
Large graft diameter preferred
-
Internal brace augmentation may be added
Posterior Cruciate Ligament
Posterior cruciate ligament grafts should be:
-
Longer
-
Larger in diameter than anterior cruciate ligament grafts
Options include:
-
Tripled semitendinosus graft
-
Allograft tissue
Internal bracing may help reduce graft elongation.
Posterolateral Corner Reconstruction
Reconstruction typically involves:
-
Fibular tunnel creation
-
Femoral tunnel placement
-
Tendon graft reconstruction of major stabilizing structures
Various reconstruction techniques exist depending on injury severity.
Medial Collateral Ligament
Management is often more conservative.
Options include:
-
Nonoperative treatment
-
Augmentation with internal brace
-
Reconstruction for severe injuries
Surgical Strategy
General intraoperative principles include:
-
Efficient surgical workflow
-
Appropriate graft preparation
-
Correct tunnel sequencing
-
Careful tensioning of reconstructed ligaments
Key Concepts
-
Multi-ligament knee injuries require systematic evaluation and management.
-
Acute management prioritizes patient survival and limb viability.
-
Early surgical reconstruction generally produces better outcomes.
-
Reconstruction is usually more reliable than isolated repair.
-
Limb alignment must be addressed in chronic instability.
Final Principle
Successful outcomes depend on optimizing every step:
-
Correct priorities
-
Accurate diagnosis
-
Proper surgical timing
-
Precise reconstruction techniques
Small improvements in each step can lead to significant improvements in overall patient outcomes.
Related Posts
-
Multi Ligament Knee Injuries
Courtesy: Chaitu Malempati, Assistant Professor, University of Kentucky, Lexington, KY, USA
-
Multi-Ligament Knee Injuries
Courtesy: Dr Peter MacDonald, FRCS, President-Elect, American Shoulder and Elbow Society, Past President, Canadian Orthopaedic…
-
Medial Collateral Ligament Injuries of Knee
Courtesy: Yogesh Joshi, Consultant Orthopaedic Surgeon, Wrexham, United Kingdom



Leave a Reply