Courtesy: Mr Fahad Hossain, Walsall NHS Healthcare, UK
Overview
-
Both unicompartmental knee arthroplasty and high tibial osteotomy preserve bone stock and native soft tissues when compared to total knee arthroplasty.
-
Both procedures provide more physiological knee kinematics and improved native proprioception relative to total knee arthroplasty.
General Indications
High Tibial Osteotomy
-
Preferred in patients younger than 55 years.
-
Suitable for patients with higher activity demands.
-
Body mass index greater than 30 kilograms per square meter is not an absolute contraindication.
-
Age greater than 55 years is not a strict contraindication when other factors favor osteotomy.
Unicompartmental Knee Arthroplasty
-
Preferred in patients older than 55 years.
-
More suitable for patients with lower activity demands.
-
Increasingly considered in younger patients with appropriate indications.
Age as a Patient Factor
High Tibial Osteotomy
-
Younger age is associated with better functional outcomes.
-
Patients older than 65 years may have inferior outcomes, but age alone should not preclude surgery if alignment and activity goals favor osteotomy.
Unicompartmental Knee Arthroplasty
-
Traditionally avoided in patients younger than 55 years due to concerns about implant longevity and higher activity levels.
-
National joint registries from Australia and the United Kingdom report higher revision rates in younger patients.
-
Recent studies demonstrate improved outcomes in younger patients when strict selection criteria and modern surgical techniques are applied.
-
Patients older than 65 years show better implant survival and lower revision rates compared to younger cohorts.
Body Habitus
High Tibial Osteotomy
-
Body mass index greater than 30 kilograms per square meter is associated with lower knee function scores but not with increased complication rates.
-
Obesity remains a negative prognostic factor for functional outcomes.
-
Lateral closing wedge osteotomy provides better inherent stability and direct bone contact in obese patients.
-
Limited comparative data exist between medial opening wedge and lateral closing wedge techniques in obese patients.
-
No significant association has been demonstrated between body mass index and conversion to total knee arthroplasty after lateral closing wedge osteotomy.
Unicompartmental Knee Arthroplasty
-
Early recommendations limited body weight to 180 pounds due to concerns regarding implant failure.
-
Contemporary evidence shows no significant differences in outcomes or implant survivorship across weight categories.
-
Meta-analyses demonstrate no increased revision risk in patients with body mass index greater than 30 kilograms per square meter at follow-up ranging from 2 to 18 years.
-
Patients with body mass index greater than 40 kilograms per square meter show similar mid-term revision rates but have a significantly higher risk of early major revision within 2 years due to mobile bearing instability and lateral compartment disease progression.
Patellofemoral Chondrosis
High Tibial Osteotomy
-
Altered joint mechanics after osteotomy may lead to progression of patellofemoral degeneration.
-
Second-look arthroscopy has demonstrated patellofemoral degeneration in up to 50 percent of patients after medial opening wedge osteotomy.
-
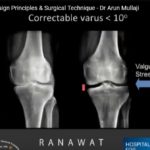
Risk factors include corrections greater than 10 degrees and valgus overcorrection.
-
Despite radiographic progression, several studies show no significant impact on clinical outcomes in the medium term.
Unicompartmental Knee Arthroplasty
-
Exposed patellofemoral subchondral bone was historically considered a contraindication.
-
Long-term studies initially identified patellofemoral disease progression as a cause of failure.
-
Modern meta-analyses demonstrate no significant difference in outcomes or revision risk in patients with patellofemoral arthritis.
-
Medial facet patellofemoral chondrosis does not adversely affect outcomes.
-
Lateral facet patellofemoral arthritis requires caution due to increased contact pressures following unicompartmental knee arthroplasty.
Anterior Cruciate Ligament Integrity
General Considerations
-
Anterior cruciate ligament injury alters knee force distribution and increases the risk of osteoarthritis within 10 years.
-
Arthritis secondary to ligament deficiency typically demonstrates a posteromedial wear pattern.
Unicompartmental Knee Arthroplasty
-
Historically contraindicated due to risks of early loosening and arthritis progression.
-
Biomechanical studies demonstrate increased contact pressures in ligament-deficient knees.
-
Short-term clinical studies show comparable survivorship and patient-reported outcomes in ligament-deficient and ligament-intact patients.
-
Long-term data remain limited, and careful patient selection is essential.
High Tibial Osteotomy
-
Outcomes are similar in ligament-deficient and ligament-intact knees.
-
Osteotomy may be combined with ligament reconstruction either as a staged or single procedure.
-
Elevated posterior tibial slope greater than 12 degrees increases stress on reconstructed ligaments.
-
Osteotomy allows correction of coronal and sagittal alignment, reducing stress on reconstructed ligaments.
-
Biplanar osteotomy with ligament reconstruction has demonstrated improved functional outcomes at mid-term follow-up.
Surgeon Factors
Unicompartmental Knee Arthroplasty
-
Revision risk decreases with increasing surgeon experience and procedural volume.
-
Surgeons performing unicompartmental knee arthroplasty in more than 30 percent of their primary knee arthroplasty cases achieve approximately 94 percent 10-year implant survival.
-
Low-volume surgeons and centers demonstrate higher revision rates compared to total knee arthroplasty.
-
High-volume centers report revision rates comparable to total knee arthroplasty.
High Tibial Osteotomy
-
Limited evidence exists linking surgeon experience or institutional volume to outcomes.
-
Large database studies demonstrate no significant association between surgeon volume, years in practice, or hospital type and conversion to total knee arthroplasty at 10 years.
Survivorship
High Tibial Osteotomy
-
5-year survivorship approximately 95 percent.
-
10-year survivorship approximately 92 percent.
-
Reported 10-year survival ranges from 75 percent to 92 percent.
-
Risk factors for failure include older age, female sex, and reduced postoperative knee flexion.
-
Modern fixation techniques show improved survivorship and reduced hardware-related complications.
-
Total knee arthroplasty after osteotomy demonstrates survivorship comparable to primary total knee arthroplasty, though the procedure is technically more demanding.
Unicompartmental Knee Arthroplasty
-
10-year survivorship ranges from 87 percent to 94 percent.
-
Implant-related failures have better outcomes than infection-related failures.
-
Common causes of revision include lateral compartment disease progression and tibial component loosening.
-
Valgus overcorrection increases the risk of lateral compartment arthritis.
-
Conversion to total knee arthroplasty is more complex than primary surgery and may require revision components.
-
Registry data suggest outcomes closer to revision total knee arthroplasty than to primary total knee arthroplasty.
Return to Activity
High Tibial Osteotomy
-
Approximately 95 percent of patients return to work at a mean of 3 months postoperatively.
-
Return to heavy labor requires longer recovery.
-
Approximately 88 percent of patients return to sports, but only 41 percent regain preoperative levels.
-
Transition to lower-impact activities is common.
Unicompartmental Knee Arthroplasty
-
Return to work rates range from 75 percent to 100 percent, most commonly between 90 percent and 95 percent.
-
Participation in high-impact sports decreases postoperatively.
-
Low- and moderate-impact recreational activities are typically maintained.
-
Patients should be counseled regarding the risks of implant wear and loosening with high-impact activities.
Summary: Procedure Selection
Factors Favoring High Tibial Osteotomy
-
Younger patient age.
-
High activity demands.
-
Mild to moderate joint space narrowing.
-
Asymmetric varus alignment.
-
Isolated anterior cruciate ligament insufficiency.
-
Need for multiplanar correction.
-
Patient preference.
Factors Favoring Unicompartmental Knee Arthroplasty
-
Older patient age.
-
Lower activity demands.
-
Advanced medial compartment osteoarthritis.
-
Acceptable mechanical alignment.
-
Absence of asymmetric varus.
-
Patient preference.
Conclusions
-
Both unicompartmental knee arthroplasty and high tibial osteotomy provide effective compartment-specific treatment for medial compartment knee osteoarthritis.
-
Both procedures preserve bone stock and native soft tissues and offer more physiological knee function than total knee arthroplasty.
-
Expanding indications for both procedures have led to significant overlap in eligible patient populations.
-
Shared decision-making between surgeon and patient is essential.
-
Patient decision aids improve understanding, reduce decisional conflict, and may represent an important future direction in selecting between unicompartmental knee arthroplasty and high tibial osteotomy.


Leave a Reply