Courtesy:Saqib Rehman MD
Epidemiology
-
Account for 11–28% of all elbow injuries
-
Posterior dislocation is most common (80–90%)
-
Annual incidence: 6–8 per 100,000 population
-
Simple dislocations: ligamentous injury only
-
Complex dislocations: associated fracture (?50%)
-
Highest incidence: 10–20 years, commonly sports-related
-
Recurrent elbow dislocation is uncommon
Anatomy of the Elbow Joint
-
A modified hinge joint with high intrinsic stability due to:
-
Joint congruity
-
Balanced muscle forces
-
Strong ligamentous constraints
-
Articulations
-
Ulnotrochlear joint – hinge motion
-
Radiocapitellar joint – rotation and valgus stability
-
Proximal radioulnar joint – forearm rotation
Elbow Stability
Anterior–Posterior Stability
-
Trochlea–olecranon fossa (extension)
-
Coronoid process
-
Radiocapitellar articulation
-
Muscle forces (biceps, triceps, brachialis)
-
Anterior joint capsule contributes to ulnohumeral stability
Valgus Stability
-
Medial Collateral Ligament (MCL) complex
-
Anterior band = primary stabilizer
-
Provides:
-
~30% valgus stability in full extension
-
50% valgus stability at 90° flexion
-
-
Resection causes gross instability except in extension
-
Varus Stability
-
Lateral Ulnar Collateral Ligament (LUCL) – static stabilizer
-
Anconeus muscle – dynamic stabilizer
Lateral Ligaments
-
Prevent posterior subluxation and rotational instability
-
Deficiency leads to posterolateral rotatory instability (PLRI)
Normal and Functional Range of Motion
-
Normal ROM
-
Flexion–extension: 0–150°
-
Supination: 85°
-
Pronation: 80°
-
-
Functional ROM
-
Flexion arc: 30–130°
-
Supination: 50°
-
Pronation: 50°
-
Mechanism of Injury
-
Most commonly due to fall on an outstretched hand (FOOSH)
-
Levering force disengages olecranon from trochlea with translation
Types by Mechanism
-
Posterior dislocation
-
Hyperextension
-
Valgus stress
-
Arm abduction
-
Forearm supination
-
-
Anterior dislocation
-
Direct blow to posterior forearm
-
Elbow in flexion
-
Capsuloligamentous Injury Pattern
-
Most elbow dislocations involve injury to all stabilizers
-
Exceptions:
-
Transolecranon fracture-dislocations
-
Large coronoid fractures
-
-
Injury progresses lateral ? medial (Horii circle)
-
Elbow may dislocate with anterior MCL band intact
-
Variable injury to common flexor and extensor origins
Clinical Evaluation
-
Guarded posture with swelling and deformity
-
Mandatory neurovascular examination:
-
Before reduction
-
After reduction
-
Serial exams if swelling is severe
-
Vascular Assessment
-
Angiography indicated if perfusion not restored post-reduction
-
Radial pulse may persist despite brachial artery injury
-
Warm, perfused hand with absent pulse ? likely arterial spasm
Additional Signs
-
Medial ecchymosis (MCL disruption) appears 3–5 days post-injury
Associated Injuries
-
Fractures
-
Radial head
-
Coronoid process
-
Capitellum / trochlea (less common)
-
-
Neurovascular
-
Ulnar nerve (most common)
-
Anterior interosseous nerve
-
Brachial artery (especially open injuries)
-
Radiographic Evaluation
-
Standard AP and lateral elbow radiographs
-
Assess:
-
Ulnohumeral congruity
-
Radiocapitellar alignment
-
-
Look for associated fractures
-
Valgus stress views (post-reduction) for MCL injury
-
CT scan for complex fracture-dislocations
Classification of Elbow Dislocations
By Complexity
-
Simple – ligamentous
-
Complex – fracture associated
By Direction of Ulna Displacement
-
Posterior
-
Posterolateral
-
Posteromedial
-
Lateral
-
Medial
-
Anterior
Fracture-Dislocations of the Elbow
Radial Head Fractures
-
Occur in 5–11%
Epicondylar Fractures
-
Occur in 12–34%
-
Can block reduction due to fragment entrapment
Coronoid Process Fractures (5–10%)
-
Usually avulsion by brachialis
Regan–Morrey Classification
-
Type I – Tip avulsion
-
Type II – ?50% of coronoid
-
Type III – >50% of coronoid
?? Fracture-dislocations have higher risk of chronic instability
Common Injury Patterns
-
Posterior dislocation + radial head fracture
-
Terrible triad:
-
Elbow dislocation
-
Radial head fracture
-
Coronoid fracture (usually Type I or II)
-
Types of Elbow Instability
-
Posterolateral rotatory instability (PLRI)
-
Varus posteromedial rotational instability
-
Olecranon fracture-dislocations
Instability Scale (Morrey)
-
Type I – LUCL injury; positive pivot shift
-
Type II – Perched dislocation; capsule + LUCL disrupted
-
Type IIIa – Posterior dislocation; posterior MCL disrupted
-
Type IIIb – Gross instability; complete MCL disruption
General Treatment Principles
-
Restore elbow stability
-
Restore trochlear notch (coronoid + olecranon)
-
Maintain radiocapitellar contact
-
LCL is more critical than MCL in most cases
-
MCL usually heals with early motion and rarely needs repair
Simple Elbow Dislocation
Non-Operative Management
-
Closed reduction under sedation/anesthesia
-
Posterior dislocations reduced in flexion with traction
-
Post-reduction:
-
Neurovascular reassessment
-
Stability assessment through ROM
-
-
Stable elbows:
-
Splint at 90°
-
Hinged brace after 3–5 days
-
-
Hinged brace for 6 weeks
-
Physical therapy after 6 weeks
-
Full recovery: 3–6 months
Closed Reduction Techniques
-
Parvin method – Prone traction, no assistant
-
Meyn & Quigley method – Forearm hanging off stretcher
Operative Indications (Simple Dislocation)
-
Instability beyond 30° flexion
-
Recurrent subluxation/dislocation
-
Associated unstable fractures
Surgical Steps
-
LCL repair first
-
MCL repair only if instability persists
-
Hinged external fixator if required
Elbow Fracture-Dislocations
Non-Operative
-
Rarely appropriate
-
High risk of stiffness and instability
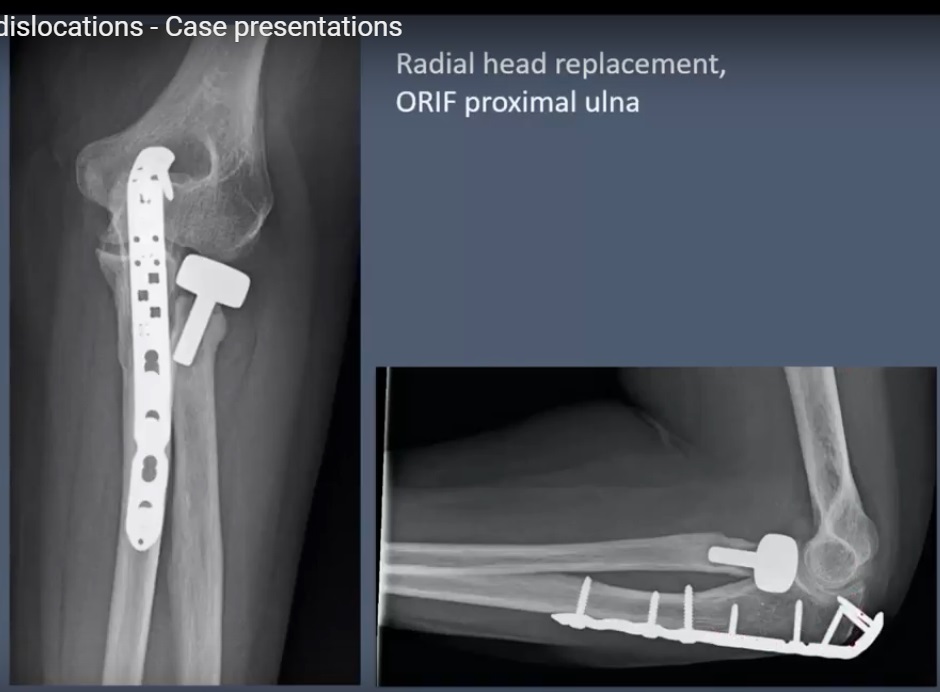
Operative Management
-
Radial head fixation or replacement
-
Coronoid fixation
-
LCL repair
-
Acute MCL repair usually not required
-
Early motion encouraged once stability restored
Terrible Triad Injuries
-
Highly unstable injury pattern
-
Requires:
-
Coronoid fixation or capsular repair
-
Radial head fixation/replacement
-
LCL repair
-
-
Radial head excision alone is contraindicated
-
External fixation or MCL repair if instability persists
Complications
-
Elbow stiffness (most common)
-
Neurologic injury
-
Ulnar nerve most frequent
-
-
Vascular injury
-
Brachial artery
-
-
Compartment syndrome
-
Persistent instability
-
Post-traumatic arthrosis
-
Heterotopic ossification
-
Increased risk with repeated manipulation
-
Avoid forceful stretching
-
Indomethacin and radiation prophylaxis are controversial
-
Key Take-Home Messages
-
Posterior elbow dislocation is most common
-
LCL is the key stabilizer in traumatic instability
-
Early, stable motion prevents stiffness
-
Fracture-dislocations require surgical management
-
Terrible triad injuries demand systematic reconstruction

Leave a Reply