Courtesy: Francesca Vannini, Rizzoli Orthopaedic Institute, Bologna, Italy
-
Background
Osteochondral lesions of the talus are increasingly encountered in clinical practice due to:
-
Rising participation in sports
-
A younger, highly active population
Treatment Goals
Management aims to:
-
Relieve pain
-
Restore cartilage (ideally hyaline-like)
-
Prevent progression to ankle osteoarthritis
Classification (Van Dijk–Based)
Acute Lesions
Lesion Size Management < 1 cm² Debridement > 1 cm² with viable fragment Fragment fixation
Chronic Lesions
Type 0
Features
-
Intact cartilage
-
Pathology confined to subchondral bone
Treatment Options
-
Retrograde drilling
-
Bone marrow aspirate concentrate (BMAC)
-
Subchondroplasty
Type 1
Features
-
Cartilage damage present
-
Lesion < 1.5 cm²
Treatment
-
Microfracture
Type 2
Features
-
Lesion > 1.5 cm²
-
Depth > 5 mm
Treatment
-
Cartilage repair or replacement
-
Bone graft or bone substitute
Type 3
Features
-
Very large lesion
-
Extensive joint surface involvement
Treatment
-
Osteochondral allograft transplantation
Pathophysiology (Van Dijk Theory)
A small defect in the subchondral bone plate leads to:
-
Joint loading forces fluid into bone
-
Increased intraosseous pressure
-
Subchondral cyst formation
-
Bone marrow edema
-
Pain
Key Insight:
Cartilage may remain intact — treatment can be directed at the subchondral bone
Subchondral Bone Treatment Options
Retrograde Drilling
Indication
-
Intact cartilage with subchondral cyst
Purpose
-
Stimulates bone healing
-
Preserves overlying cartilage
Bone Marrow Aspirate Concentrate (BMAC)
Technique
-
Bone marrow aspirated (usually posterior iliac crest)
-
Concentrated and injected under imaging guidance
Benefits
-
Provides mesenchymal stem cells
-
Enhances bone healing
Subchondroplasty
Method
-
Injection of calcium phosphate bone substitute
Advantages
-
Provides structural support
-
Acts as a biological scaffold
Indications
-
Bone marrow edema
-
Subchondral cysts
Cartilage Repair Techniques
Autologous Chondrocyte Implantation (ACI)
Procedure
-
Cartilage biopsy
-
Cell culture
-
Implantation under periosteal flap
Advantages
-
Suitable for large lesions
-
Produces hyaline-like cartilage
Disadvantages
-
Two-stage procedure
-
Expensive
Matrix-Induced Autologous Chondrocyte Implantation (MACI)
Concept
-
Chondrocytes embedded in a collagen scaffold
-
Implanted arthroscopically
Advantages
-
Less invasive than ACI
-
Improved cell distribution and support
Bone Marrow–Derived Cell Transplantation
Steps
-
Harvest bone marrow
-
Concentrate cells
-
Load onto scaffold
-
Arthroscopic implantation
-
Cover with platelet-rich gel
Advantages
-
Single-stage procedure
-
Cost-effective
-
Good clinical outcomes
Important Associated Factors
Successful treatment requires addressing:
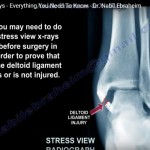
Ligament Stability
-
Instability must be corrected
Failure leads to poor outcomes
Alignment
-
Malalignment adversely affects results
Corrective Procedures
-
Fibular lengthening
-
Supramalleolar osteotomy
Arthritis
-
Presence and severity influence prognosis
Rehabilitation Protocol
Phase 1 (0–8 Weeks)
-
Non-weight bearing for 6 weeks
-
Begin:
-
Pool exercises
-
Cycling
-
-
Gradual partial weight bearing after 8 weeks
Phase 2 (16 Weeks Onwards)
Assessment
-
Gait
-
Proprioception
Progression
-
If normal — light running
-
If pain/swelling — continue physiotherapy
Return to Sports
-
Directional training: ~6 months
-
Full sports activity: ~8 months
Osteochondral Allograft (Large Lesions)
Indications
-
Massive talar dome defects
Advantages
-
Restores both:
-
Bone
-
Cartilage
-
-
No donor site morbidity
Disadvantages
-
High cost
-
Difficulty in graft matching
-
Risk of immune reaction
-
Prolonged rehabilitation
Types
Partial Allograft
-
For localized talar dome lesions
Bipolar Allograft
-
Replaces both:
-
Tibial surface
-
Talar surface
-
Indication
-
Severe ankle arthritis
Complications
-
Graft malposition
-
Failure due to early weight bearing
-
Recurrence of arthritis
-
Immunologic reaction
Postoperative Consideration
-
Often requires prolonged non-weight bearing (~6 months)
Key Takeaways
-
OLT incidence is increasing in young active patients
-
Treatment depends on:
-
Lesion size
-
Cartilage status
-
Depth
-
-
Subchondral bone is a key pain generator
-
Always correct:
-
Instability
-
Malalignment
-
-
Large lesions may require osteochondral allograft
-
Rehabilitation is prolonged and crucial for outcomes
-


Leave a Reply