Live Webinar Hosted on Orthopaedic Principles
Prevalence of Ankle Fractures
-
Incidence ranges from 4.2 to 18.7 per 10,000 person-years.
-
Account for approximately 9% of fractures treated in orthopaedic trauma.
-
Demonstrate a bimodal age distribution:
-
Higher incidence in young men
-
Increased incidence in adults older than 50 years
-
-
Approximately 25% to 50% of ankle fractures require surgical intervention.
Increased Risk and Challenges with Age and Diabetes
-
Risk of ankle fractures increases significantly after the age of 50 years.
-
Diabetic patients sustain higher complication rates following ankle fractures, irrespective of whether treatment is surgical or nonsurgical.
-
Complication risk is particularly elevated in patients with:
-
Diabetic neuropathy
-
Peripheral vascular disease
-
-
Common complications include:
-
Failure of fixation
-
Malunion
-
Wound infection
-
Limb loss
-
Physiological Considerations in Diabetes
-
Diabetes is frequently associated with comorbidities such as smoking, obesity, hypertension, and chronic kidney disease, all of which increase complication risk.
-
Diabetes mellitus is a metabolic disorder characterized by chronic hyperglycemia and includes:
-
Type 1 diabetes
-
Type 2 diabetes, which accounts for approximately 90% of cases
-
-
Persistent hyperglycemia causes tissue damage through:
-
Protein glycosylation
-
Formation of advanced glycation end products
-
Accumulation of intracellular sorbitol and other polyols
-
Increased oxidative stress
-
-
These mechanisms lead to:
-
Neuropathy
-
Microangiopathy
-
Macroangiopathy
-
Immune dysfunction
-
-
These physiological changes significantly increase complication rates in ankle fractures.
Glucose Control and Surgical Risk
-
Insulin dependence in type 2 diabetes is commonly used as a marker of disease severity and glycemic control.
-
Insulin-dependent diabetes is associated with higher complication rates following ankle fracture surgery compared with non-insulin-dependent diabetes.
-
Studies demonstrate higher rates of:
-
Amputation
-
Infection
-
Reoperation
-
Readmission
-
Surgical site infection
-
Osteomyelitis
-
Wound dehiscence
-
Bleeding
-
Sepsis
-
Mortality
-
-
Hemoglobin A1c reflects average blood glucose levels over the preceding 3 months.
-
Hemoglobin A1c values greater than 6.5% are associated with increased complication rates.
-
No definitive threshold value has been established, but rising levels correlate with poorer radiographic and functional outcomes.
-
In patients with severely elevated hemoglobin A1c or uncontrolled glucose levels, a multidisciplinary perioperative approach involving endocrinology and anesthesia is essential.
Diabetic Neuropathy
-
Diabetic peripheral neuropathy significantly increases complication risk in ankle fractures.
-
Prevalence:
-
Approximately 21% within 5 years of diabetes onset
-
Up to 41% within 10 years
-
-
Loss of protective sensation increases ulcer risk:
-
3-fold with reduced sensation
-
9-fold with absent sensation
-
-
Loss of vibratory sensation is a sensitive indicator of neuropathy and increases ulcer risk by 7-fold.
-
Autonomic neuropathy occurs in 30% to 50% of patients with sensory neuropathy and leads to:
-
Dry, cracked skin
-
Increased ulcer risk by approximately 4-fold
-
-
Diagnostic evaluation:
-
Nerve conduction studies are the gold standard
-
Common clinical screening tools include Semmes–Weinstein monofilament testing and a 128-hertz tuning fork
-
-
Routine neuropathy screening is essential in diabetic patients with ankle fractures.
Diabetic Vasculopathy
-
Diabetic patients have increased risk of both macrovascular and microvascular disease.
-
Peripheral arterial disease is approximately twice as common in diabetics compared with the general population.
-
Reported prevalence ranges from 20% to 50%.
-
Microvascular dysfunction is influenced by impaired neurovascular and neurogenic control.
-
Vascular assessment includes:
-
Ankle brachial index
-
Toe brachial index
-
-
Both tests should be used together, as calcified, noncompressible arteries may falsely elevate ankle brachial index values.
-
Suspected vascular compromise warrants vascular surgery consultation to assess healing potential and the need for revascularization.
Delayed Healing in Diabetes
-
Diabetes adversely affects both soft-tissue and bone healing.
-
Experimental studies demonstrate:
-
Reduced collagen synthesis
-
Weakened callus formation
-
-
Chronic hyperglycemia and advanced glycation end products impair osteoblast differentiation.
-
Diabetes promotes a chronic inflammatory state with elevated proinflammatory cytokines, leading to:
-
Impaired granulation tissue formation
-
Reduced wound tensile strength
-
-
These host-related factors complicate ankle fracture management in diabetic patients.
Nonoperative Management
-
There are no randomized or prospective studies evaluating nonoperative versus operative treatment of ankle fractures in diabetic patients.
-
Available evidence is limited to retrospective studies.
Evidence from Retrospective Studies
-
Lovy et al. evaluated displaced ankle fractures in diabetic patients:
-
Nonoperative group: 75% complication rate
-
Complications included loss of reduction, Charcot arthropathy, cast-related ulcers, reoperation, and deep infection
-
Operative group: 12.5% complication rate
-
Operative fixation after failed nonoperative care resulted in a 100% complication rate
-
Recommendations
-
Unstable ankle fractures in diabetic patients should generally be treated operatively with anatomic reduction and rigid fixation.
-
Stable fractures may be treated nonoperatively with close monitoring for skin breakdown and ulceration.
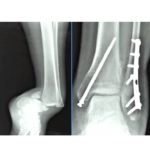
Operative Techniques and Considerations
Open Reduction and Internal Fixation
-
Reported complication rates in diabetic patients range from 14% to 36%.
-
Infection rates range from 12% to 36%, with deep infection rates of 7% to 10%.
-
Increased complication risk is associated with absent pedal pulses and peripheral vascular disease.
-
Functional outcomes may be inferior in diabetic patients compared with nondiabetic patients.
Supplemental Stabilization
-
Augmentation with transarticular or trans-calcaneal fixation may improve construct stability.
-
Supplemental fixation has been associated with reduced complication rates in select patient populations.
Fixation Strategies
-
Locking plates
-
Posterior antiglide plates
-
Direct fixation of posterior malleolar fragments
-
Trans-syndesmotic fixation
-
Increased construct stiffness and fixation density are often required to compensate for poor bone quality and delayed healing.
Minimally Invasive Surgical Techniques
-
Diabetic patients are at increased risk of wound complications, encouraging the use of less invasive approaches.
Techniques Include
-
Minimally invasive plate fixation with smaller incisions and reduced soft-tissue disruption
-
Percutaneous cannulated screw fixation
-
Intramedullary fibular nail fixation for rotational ankle injuries
-
Primary arthrodesis using tibiotalocalcaneal nails as a salvage procedure, with or without formal joint preparation
-
These techniques offer improved construct rigidity with less soft-tissue compromise.
-
Arthroscopy may be used to assess cartilage injury and confirm fracture reduction.
Additional Considerations
-
Equinus contracture should be evaluated in diabetic patients.
-
Gastrocnemius or Achilles tendon lengthening may be required to reduce forefoot or midfoot ulcer risk.
Wound Care and Infection Prevention
-
Vacuum-assisted closure has been shown to reduce surgical site infection rates compared with standard moist wound care.
-
Practical limitations include difficulty with application, interference with immobilization, and need for specialized nursing care.
-
Topical vancomycin powder applied intraoperatively has been shown to reduce deep infection rates and may be considered in high-risk patients.
Postoperative Care
-
Delayed bone healing is common, necessitating prolonged protected weight bearing.
-
Immobilization for up to 8 weeks has traditionally been recommended.
-
Recent evidence supports earlier protected weight bearing when stable fixation and load-sharing devices are used.
-
Prolonged non-weight bearing may result in significant morbidity, especially in patients unable to use assistive devices.
-
Optimal rehabilitation protocols remain an area for future research.
Complications
-
Diabetic patients with ankle fractures have significantly higher risks of:
-
Infection
-
Nonunion
-
Malunion
-
Revision surgery
-
Amputation
-
-
Infection risk is increased 4.7-fold in diabetes and further amplified by neuropathy.
-
Complicated diabetes carries:
-
6-fold higher infection risk compared with uncomplicated diabetes
-
10-fold higher risk compared with nondiabetic patients
-
-
Management often requires a multidisciplinary team including orthopaedics, endocrinology, infectious disease, vascular surgery, and wound care specialists.
-
Severe cases may require staged reconstruction or amputation.
Conclusion
-
Operative treatment is generally recommended for unstable ankle fractures in diabetic patients.
-
Enhanced fixation strategies or intramedullary fixation should be considered in patients with complicated diabetes.
-
Thorough counseling of patients and families is essential to explain the elevated risk of complications, including limb loss


Leave a Reply