Courtesy: Lyndon Mason, FRCSOrth, Liverpool, UK
Achilles Tendon Rupture – Key Orthopaedic Principles
Introduction
- The Achilles tendon is formed by:
- Gastrocnemius
- Soleus
- (Together called triceps surae)
Insertion
- Calcaneal tuberosity
Fiber Orientation
- Tendon fibers rotate before insertion
- Medial gastrocnemius fibers insert more posteriorly
Clinical Note
- Medial gastrocnemius release can improve tightness
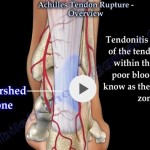
Blood Supply
Segmental Supply
- Proximal – Posterior tibial artery
- Distal – Posterior tibial artery
- Mid-portion – Peroneal artery
Key Point
- Mid-portion has:
- Least vascularity
- Most common rupture site
Epidemiology
- Incidence: 6–10 per 100,000
- ~75% occur during sports
Demographics
- More common in:
- Males
- Middle-aged individuals
“Weekend Warrior” Phenomenon
- Sedentary lifestyle + sudden intense activity
Risk Factors
Intrinsic
- Tendon degeneration
- Reduced vascularity
- Aging
Extrinsic
- Overuse
- Sudden eccentric contraction
- Sudden increase in activity
Medical Conditions
- Rheumatoid arthritis
- Gout
- Ankylosing spondylitis
Medications
- Fluoroquinolones
- Phenytoin
Pathophysiology
- Most ruptures occur in:
- Degenerated tendon
Mechanism
- Strain > 8% elongation
Typical Injury
- Eccentric loading of plantarflexed ankle
Clinical Presentation
Classic History
- “Hit at the back of the leg”
- Sudden pop or snap
- Immediate inability to continue activity
Common Activities
- Football
- Running
- Dancing
Clinical Examination
Inspection
- Swelling
- Loss of tendon contour
Palpation
- Possible palpable gap
Special Test
Thompson Test (Simmonds Test)
- Patient prone – calf squeezed
Interpretation
- Normal – plantarflexion
- Rupture – no plantarflexion
Imaging
X-ray
- May show:
- Loss of Kager’s fat pad
Ultrasound
- Useful but not always required
MRI
- Indications:
- Chronic rupture
- Surgical planning
Tendon Gap Concept
- Earlier belief:
- Gap >1 cm – poor outcome
Current Understanding
- Tendon tears are:
- Irregular (“seaweed tear”)
Conclusion
- Gap measurement:
- Not clinically reliable
Healing Biology
Early Phase
- Type I collagen – after 3 days
First 2 Weeks
- Type III collagen predominates
After 2 Weeks
- Collagen reorganizes longitudinally
Definitions
- Acute rupture – <2 weeks
- Chronic rupture – >2 weeks
Rehabilitation Principles
- Controlled loading improves healing
Problems with Immobilization
- Weak scar formation
Benefits of Early Mobilization
- Better collagen alignment
- Stronger tendon
Treatment
1. Non-Operative (Preferred)
Modern Functional Rehabilitation
- Functional boot
- Early mobilization
- Gradual weight bearing
Outcomes
- Re-rupture rate:
- <1%
- Comparable to surgery
Orthotic Consideration
- Boot must provide:
- True equinus position
Important
- Flat boots may:
- Fail to shorten tendon properly
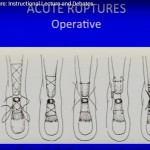
2. Surgical Treatment
Indications
- Failed conservative treatment
- Chronic rupture
- Insertional rupture
- Elite athletes (selected)
- Delayed diagnosis
Complications (10–15%)
- Infection
- Wound problems
- Nerve injury
- Re-operation
Minimally Invasive Surgery
- No clear functional advantage
Deep Vein Thrombosis (DVT)
- Highest risk among foot & ankle injuries
Incidence
- Up to 50% (screened cases)
Important
- Risk persists regardless of:
- Treatment type
- Weight bearing
Return to Sport
- Return rate:
- 65–100%
Time Frame
- 3–13 months
Elite Athletes
- ~60% return
Psychological Factors
- Fear of re-rupture
- Fear of movement
- Lack of confidence
Clinical Insight
- Psychological readiness affects recovery
Chronic Achilles Tendon Rupture
Definition
- Rupture >2–4 weeks
Treatment Based on Gap
| Gap Size | Treatment |
|---|---|
| <2 cm | Primary repair |
| 2–5 cm | V-Y advancement |
| >5 cm | Tendon transfer / graft |
Surgical Options
1. V-Y Gastrocnemius Advancement
- For moderate defects
2. Tendon Transfer
Common Choice
- Flexor hallucis longus (FHL)
Advantages
- Strong plantarflexor
- Anatomically close
- Easy access
3. Tendon Grafts
- Autograft
- Allograft (e.g., semitendinosus)
Preferred Reconstruction Strategy
- FHL transfer
- Resection of degenerated tendon
- Allograft reconstruction
Benefits
- Restores tension
- Biological support
- Good functional outcome
Key Takeaways
- Common in middle-aged recreational athletes
- Diagnosis is clinical (Thompson test)
- Functional rehab often preferred over surgery
- Surgery has higher complication risk
- Chronic ruptures require reconstruction
- Psychological factors strongly influence outcomes


Leave a Reply