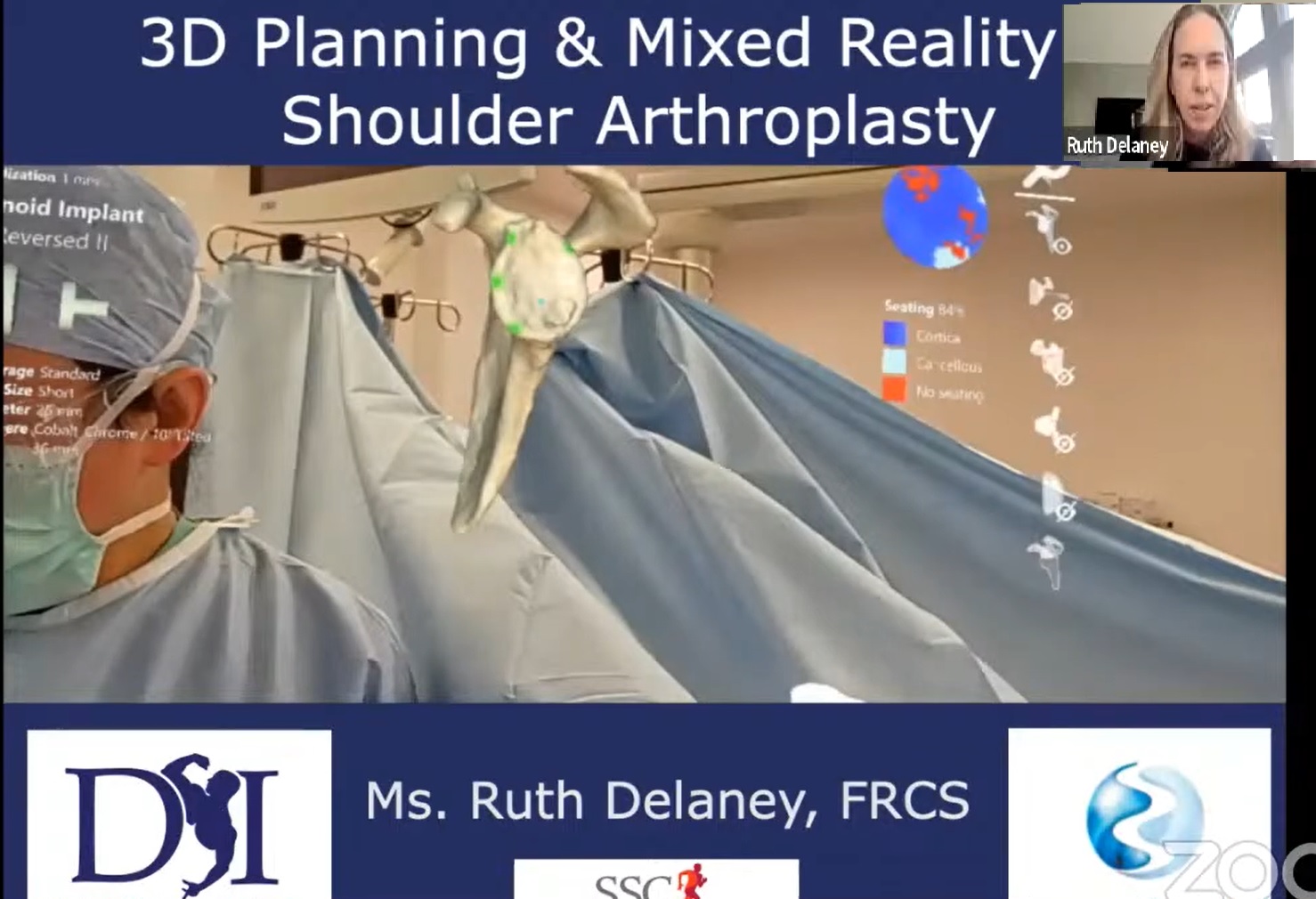
Courtesy: Ms. Ruth Delaney, MB BCh, MMedSc, FFSEM, FRCS
Founder, Dublin Shoulder Institute
Consultant Orthopaedic Surgeon, Shoulder Surgery Specialist, Associate Professor
Introduction to Mixed Reality
What Is Mixed Reality?
-
Mixed reality is a technology that blends the real physical world with digitally generated content.
-
It allows surgeons to interact with virtual objects while remaining aware of the real environment.
-
The concept was first described in 1994 by Paul Milgram, who placed mixed reality along a continuum between the real world and fully virtual environments.
Reality–Virtuality Continuum
-
Real world
-
Augmented reality
-
Mixed reality
-
Virtual reality
Key Mixed Reality Devices Used in Surgery
-
Microsoft HoloLens
-
Introduced in 2017
-
Head-mounted mixed reality device used for surgical visualization, navigation, and training
-
-
Magic Leap
-
Advanced spatial computing headset
-
Enables three-dimensional holographic visualization and interaction
-
Market Growth and Relevance
-
The global augmented reality and virtual reality market is projected to grow by approximately three hundred and fifty percent.
-
Market value is expected to increase from two point seven billion United States dollars to nearly ten billion United States dollars over the next five years.
-
This rapid growth highlights increasing adoption in healthcare and surgical practice.
How Mixed Reality Works in Surgery
Head-Mounted Display Technology
-
Sterile, hands-free holographic visualization within the operating room
-
Interaction through:
-
Voice commands
-
Hand and gesture controls
-
Three-Dimensional Planning and Navigation
-
Integration of preoperative imaging such as:
-
Computed tomography scans
-
Magnetic resonance imaging scans
-
-
Real-time intraoperative guidance with holographic overlays
Why Mixed Reality in Upper Extremity Surgery?
Challenges in Upper Extremity Procedures
-
Highly complex anatomy involving:
-
Nerves
-
Blood vessels
-
Small and irregular bones
-
-
Requirement for extreme precision in procedures such as:
-
Glenoid component placement
-
Corrective osteotomies
-
Mixed Reality Solutions
-
Enhanced three-dimensional anatomical visualization
-
Real-time intraoperative adjustments based on patient-specific anatomy
Preoperative Applications
-
Three-dimensional fracture mapping:
-
Scapula fractures
-
Humerus fractures
-
-
Virtual implant sizing and positioning
-
Surgical rehearsal and simulation prior to entering the operating room
Intraoperative Applications
-
Live navigation for critical steps such as:
-
Glenoid guide pin placement
-
-
Holographic surgical guides:
-
Kirschner wire trajectory visualization
-
-
Remote collaboration:
-
Real-time expert input during surgery
-
General Benefits of Mixed Reality in Orthopaedic Trauma
-
Provides intuitive real-time feedback to improve:
-
Implant positioning accuracy
-
Surgical efficiency
-
-
Clinical studies demonstrate:
-
Reduced operative time
-
Decreased radiation exposure
-
Improved accuracy in procedures such as:
-
Superior pubic ramus Kirschner wire placement
-
Dynamic hip screw insertion
-
-
Trauma Applications
Proximal Humerus Fractures
-
Clinical challenge:
-
Complex fracture patterns
-
-
Mixed reality solution:
-
Virtual fracture reduction planning
-
Guidance for percutaneous pin placement
-
Elbow Stabilization Using an Internal Joint Stabilizer
-
Clinical challenge:
-
Accurate drilling along the transepicondylar axis
-
-
Mixed reality solution:
-
Holographic alignment of the anatomical axis
-
Osteotomy Applications
Cubitus Varus Deformity Correction
-
Clinical challenge:
-
High complication rates
-
-
Mixed reality solution:
-
Virtual wedge planning
-
Real-time intraoperative adjustment
-
Arthroplasty Applications
Reverse Shoulder Arthroplasty
-
Clinical challenge:
-
Malpositioning of the glenoid component
-
-
Mixed reality solution:
-
Three-dimensional preoperative planning
-
Live intraoperative navigation
-
Arthroscopy Applications
Rotator Cuff Repair
-
Clinical challenge:
-
Optimal portal placement
-
-
Mixed reality solution:
-
Virtual humerus rotation to improve footprint access
-
Glenoid Reconstruction for Shoulder Instability
-
Clinical challenge:
-
Significant bone loss
-
-
Mixed reality solution:
-
Holographic shaping of distal tibia allograft
-
Acromioclavicular Joint Injury Repair
-
Clinical challenge:
-
Coracoid drilling accuracy with conventional techniques ranges from sixty-two to eighty-four percent
-
-
Mixed reality advantages:
-
Improved spatial awareness
-
Virtual drill guides replicating ideal clavicle-to-coracoid trajectory
-
Holographic measurements for precise positioning
-
Virtual screens displaying fluoroscopy and arthroscopic views
-
Oncology Applications
Tumor Resection
-
Clinical challenge:
-
Tumor proximity to nerves and blood vessels
-
-
Mixed reality solution:
-
Three-dimensional tumor visualization
-
Mapping of adjacent neurovascular structures
-
Remote Collaboration and Surgical Training
-
Live surgical streaming for expert guidance during procedures
-
Resident and fellow training through immersive virtual simulations
-
Enhanced understanding of complex anatomy without patient risk
Benefits of Mixed Reality in Surgery
-
Increased precision, with reported accuracy within approximately one millimeter
-
Reduced radiation exposure due to decreased fluoroscopy use
-
Faster procedures, with time reductions of up to twenty percent
-
Improved surgical education and training outcomes
Challenges and Limitations
-
High initial costs for hardware and software
-
Learning curve for surgeons and operating room staff
-
Potential technical issues during surgery
-
Increased preoperative planning time
Future Directions
-
Integration of artificial intelligence for automated planning and decision support
-
Development of smaller, lighter, and more affordable devices
-
Wider adoption across operating rooms and surgical specialties
Conclusion
-
Mixed reality represents a major advancement in upper extremity surgery.
-
It significantly improves surgical precision, efficiency, and collaboration.
-
Ongoing research is required to establish long-term outcomes and cost-effectiveness.
-
With continued technological evolution, mixed reality is likely to become an integral part of modern orthopaedic practice.




Leave a Reply